Band ligation for a gastroesophageal junction Dieulafoys lesion
Mohammed Amine Benatta, Jean Charles Grimaud
PAMJ. 2017; 26:181. Published 29 Mar 2017 | doi:10.11604/pamj.2017.26.181.9747
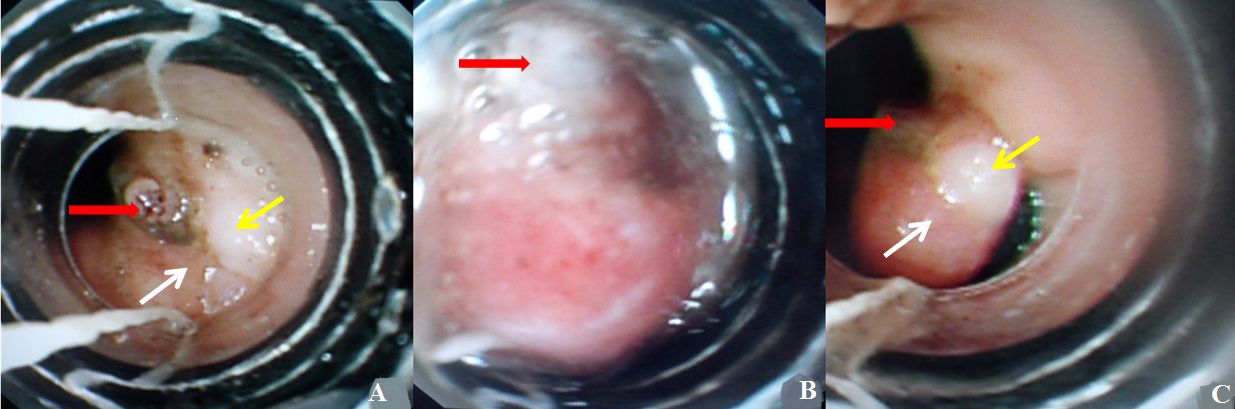
Corresponding author
Mohammed Amine Benatta, Digestive Endoscopy Unit, Central Hospital of Army (HCA), Algiers, Algeria (benattaamine@yahoo.fr)
This image
| Articles published in PAMJ are Open Access and distributed under the terms of the Creative Commons Attribution 4.0 International (CC BY 4.0). |  |
eISSN: 1937-8688
The Pan African Medical Journal (ISSN: 1937-8688) is a subsidiary of the Pan African Medical Journal. The contents of this journal is intended exclusively for professionals in the medical, paramedical and public health and other health sectors.
Currently tracked by: DOAJ, AIM, Google Scholar, AJOL, EBSCO, Scopus, Embase, IC, HINARI, Global Health, PubMed Central, PubMed/Medline, ESCI
Physical address: "Kenya: 3rd Floor, Park Suite Building, Parkland Road, Nairobi. PoBox 38583-00100, tel: +254 (0)20-520-4356 | Cameroon: Immeuble TechnoPark Essos, Yaounde, PoBox: 10020 Yaounde, tel: +237 (0)24-309-5880"





