Uncommon mimics of appendicitis: giant mucocele
Fatima Ezzahra Zahid, Karim Ibn Majdoub, Hicham Anoune, Abdelmalk Ousadden, Khalid Mazaz, Khalid Ait Taleb
Corresponding author: Department of General Surgery, CHU Hassan II Fes, Morocco 
Received: 03 Oct 2010 - Accepted: 30 Sep 2010 - Published: 21 Oct 2010
Domain: Surgery
Keywords: Abdominal pain, appendicitis, mucocele, complication, malignancy, Morocco
©Fatima Ezzahra Zahid et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Fatima Ezzahra Zahid et al. Uncommon mimics of appendicitis: giant mucocele. Pan African Medical Journal. 2010;7:7. [doi: 10.11604/pamj.2010.7.7.355]
Available online at: https://www.panafrican-med-journal.com//content/article/7/7/full
Uncommon mimics of appendicitis: giant mucocele
Fatima Ezzahra Zahid1,&, Karim Ibn Majdoub1, Hicham Anoune1, Abdelmalk Ousadden1, Khalid Mazaz1, Khalid Ait Taleb1
1Department of General Surgery, CHU Hassan II Fes, Morocco
&Corresponding author
Fatima Ezzahra Zahid, Department of General Surgery, CHU Hassan II Fes, Morocco
Abdominal pain is one of the most common presenting complaints evaluated in the Emergency Department (ED). Acute right lower quadrant (RLQ) pain comprises a significant number of these presentations. A broad spectrum of common and uncommon entities may mimic acute appendicitis. Uncommon mimics include mucocele. We present a case of acute, right lower quadrant discomfort in which appendiceal mucocele was an incidental finding in the operation for acute appendicitis and discuss the pathology, associated complications, evaluation and treatment of this uncommon, but important finding. Histopathological analysis demonstrated a mucinous cystadenoma.
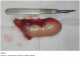
Our patient was fiftyfive year-old male who presented with complaints of acute right lower quadrant pain, nausea and vomiting. Written permission was obtained from the patient before the publication of this case report and accompanying images. Physical examination revealed mild tenderness, right lower quadrant pain upon palpation, muscular rigidity and rebound tenderness. White blood cell count was 16000 elements/ mm3 and other laboratory values were normally. An emergency operation was performed for acute appendicitis, but an enflame mobile cystic mass with 10x7 cm in its great dimension was observed in the right iliac fossa. During the operation a diagnosis of a mucocele of the appendix was made (figure 1). Surgical treatment included only appendectomy. Histopathological analysis demonstrated a mucinous cystadenoma.
Appendiceal mucocele is an uncommon abnormality, first described by Rokitansky [1]. It�s a general macroscopic description that implies a dilated appendiceal lumen caused by an abnormal accumulation of mucus. The term does not indicate etiology and includes both benign and malignant entities [1,2]. The underlying pathology can be subdivided into 4 histologic types: mucinous cystadenoma (63%), mucosal hyperplasia (25%), mucinous cystadenocarcinoma (11%) and retention cyst [3]. Mucocele can also occur due to occlusion of the lumen by endometriosis or carcinoid tumour.
The clinical presentation of appendiceal mucoceles is often nonspecific. Most
mucoceles are asymptomatic, and as many as 50% are found incidentally during
radiological evaluations, endoscopic procedures or surgery [1].
The most common presentation of symptomatic AM patients is acute or chronic
right lower quadrant abdominal pain, as occurred with our patient. Cyclical or
colicky pain can occur when AM is associated with intussusception or
endometriosis. An intra-abdominal mass is palpated by the examining physician
in half of cases and is also occasionally palpated by the patient. Nausea and
vomiting, as well as altered bowel habits (e.g., diarrhea, constipation) are
often reported, and evidence of gastrointestinal bleeding is noted if intussusception
is present [3,4]. The average age at
diagnosis is 50 years and, although early reports suggested that AM occurred
more frequently in women than men, this predominance has been challenged in
more recent studies [1].
The initial detection of the lesion may be facilitated by radiological,
sonographic or endoscopic means. Ultrasound findings can be variable. Purely
cystic lesions with anechoic fluid, hypoechoic masses with fine internal echoes
as well as complex hyperechoic masses can be seen depending on the contents [4]. The onion skin sign is considered to be specific for
mucocele of the appendix [5]. CT of the abdomen usually
shows a cystic well-encapslated mass sometimes with mural calcification, in the
expected location of the appendix. It may be causing extrinsic pressure on the
caecal wall without any surrounding inflammatory reaction [2,6,7]. Magnetic resonance imaging has
been reported useful for the evaluation of AM and also has the advantage of
demonstrating any concomitant pathology [1]. In most
instances, a correct pre-operative diagnosis of AM can be made with the
combined use of US and CT scan [4]. On barium enema, there
is usually non filling or partial filling of the appendix with contrast. The
lesion may be seen as a sharply outlined sub mucosal or extrinsic mass
indenting the caecum and laterally displacing it [8].
Colonoscopic findings include the �volcano sign�, the appendiceal orifice seen
in the centre of a firm mound covered by normal mucosa or a yellowish,
lipoma-like submucosal mass [8].
The treatment of cystic appendiceal masses is primarily surgical excision. It can either be by laparotomy or laparoscopy. Laparoscopic surgery provides the advantages of good exposure and evaluation of entire abdominal cavity, as well as more rapid recovery with avoidance of a large incision and a better cosmetic outcome. However careful handling of the specimen is recommended as spillage of the contents can lead to pseudomyxoma peritonei. This can be achieved by atraumatic handling of the appendix and use of impermeable bag for removal of the specimen. Conversion to laparotomy should be considered if the lesion is traumatically grasped or if the tumour clearly extends beyond the appendix or if there is evidence of malignancy such as peritoneal deposits [9]. Some suggest that a frozen-section examination should be performed while the abdomen is open [2].
Involvement of the caecum or adjacent organs is an indication for right hemi-colectomy and thorough exploration of the gastrointestinal tract and ovaries [10]. Patients with a simple or benign neoplastic mucocele have an excellent postoperative prognosis, with 5-year survival rates of 91%�100%, even in cases of extension of mucus into the extra-appendiceal spaces. However, the clinical course of diffuse pseudomyxoma peritonei is insidious and unrelenting [2]. When a mucocele is present, associated neoplasms of the gastrointestinal tract, breast, ovary, and kidney must also be considered; associated colonic tumours are the most common reported.
Mucocele is an uncommon pathology of the vermiform appendix that can be confused with acute appendicitis. They are difficult to diagnose and are usually discovered incidentally during operation. Appendectomy is usually sufficient; however, if the mass extends into the cecum, a right hemicolectomy may be required.
Figure 1: specimen of appendicectomy showing an enlarged appendice
The authors declare that they have no competing interests.
Fatima ezzahra Zahid is a surgeon who drafted the manuscript and revised it critically for content. Karim Ibn Majdoub, Hicham Anoune are surgeons who are involved in literature research. Khalid Mazaz and Khalid A�t Taleb are surgeons treating of the patient and were involved in revising the draft critically for content. Abdelmalek Ousadden is a surgeon was get photographs and was involved in drafting the manuscript. All authors have given final approval of the revision to be published.
- Ciprian Bartlett, Madhavi Manoharan, Anne Jackson. Mucocele of the appendix � a diagnostic dilemma: a case report. Journal of Medical Case Reports. 2007; 1:183. This article on PubMed
- Jim�nez Mazure C, Ram�rez Plaza CP, Valle Carbajo M, Santoyo Santoyo J. Giant appendiceal mucocele:Implications for diagnosis and therapeutic. Rev Esp Enferm Dig. 2009 Jun;101(6):447-9. This article on PubMed
- Fairise , Barbary , Derelle , Tissier , Granger , Marchal , Laurent , Regent. Mucoc�le pendiculaire et pseudomyxome p�riton�al. J Radiol. 2008; 89:751-762. This article on PubMed
- Roberto Gibson Ferreira Costa. Mucocele of the appendix. Rev Col Bras Cir. 2009; 36(2):180-182. This article on PubMed
- Chou JW, Feng CL, Lai HC. Appendiceal mucocel presenting with lower abdominal pain. Endoscopy. 2009;41 Suppl 2:E222-3. This article on PubMed
- Gillion JF, Franco D, Chapuis O, Serpeau D, Convard JP, Jull�s MC, Balaton A, Karkouche B, Capelle P, Parmentier T, Chollet JM, Thillois JM, Berthelot G. Appendiceal mucoceles, pseudomyxoma peritonei, and appendicel mucinous neoplasms: update on contribution of imaging to choice of surgical approach. J Chir (Paris). 2009 Apr;146(2):150-66. This article on PubMed
- Persaud T, Swan N, Torreggiani WC. Giant mucinous cystadenoma of the appendix. Radiographics. 2007 Mar-Apr;27(2):553-7. This article on PubMed
- Tynan JR, Marshall GB, Gray RR. Answer to Case of the month #107 Appendiceal Mucocele as a Presentation of Mucinous Adenocarcinoma. Can Assoc Radiol J. 2006 Apr;57(2):117-9. This article on PubMed
- Rangarajan Palanivelu, Kavalakat Parthasarathi. Laparoscopic appendectomy for mucocele of the appendix: report of 8 cases. Indian J Gastroenterol. 2006; 25: 256-257. This article on PubMed
- Roberge RJ, Park AJ. Mucocele of the appendix: an important clinical rarity. J Emerg Med. 2006 Apr;30(3):303-6. This article on PubMed