Sneddon syndrome
Hakima Elmahi, Fatima Zahra mernissi
Corresponding author: Hakima Elmahi, Department of Dermatology, University Hospital Hassan II, Fez, Morocco 
Received: 05 Feb 2017 - Accepted: 07 Mar 2017 - Published: 04 Sep 2019
Domain: Health communication
Keywords: Sneddon syndrome, skin disease, antiphospholipid antibodies
©Hakima Elmahi et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Hakima Elmahi et al. Sneddon syndrome. Pan African Medical Journal. 2019;34:9. [doi: 10.11604/pamj.2019.34.9.11903]
Available online at: https://www.panafrican-med-journal.com//content/article/34/9/full
Sneddon syndrome
Hakima Elmahi1,&, Fatima Zahra Mernissi1
1Department of Dermatology, University Hospital Hassan II, Fez, Morocco
&Corresponding author
Hakima Elmahi, Department of Dermatology, University Hospital Hassan II, Fez, Morocco
Sneddon's syndrome (SS) is a rare non-inflammatory thrombotic vasculopathy characterized by the combination of cerebrovascular disease with livedo racemosa(LR). It has been estimated that the incidence of SS is 4 per 1 million per annum in general population and generally occurs in women between the ages of 20 and 42 years. Approximately 80% of Sneddon's syndrome patients have an antiphospholipid antibody marker. LR may precede the onset of stroke by years and the trunk and/or buttocks are involved in nearly all patients. The cerebrovascular manifestations are mostly secondary to ischemia (transient ischemic attacks and cerebral infarct). Other neurological symptoms range from headache, cerebral hemorrhage, seizures, cognitive and psychiatric disturbances. The involved internal organs include heart, kidney, and eyes. Histological findings of skin are characteristic and the involved vessels are small to medium-sized arteries at the border of dermis to subcutis with a distinct histopathological time course. The main diagnostic criteria are general LR with typical histopathological findings on skin biopsy and focal neurological deficits. The pathogenesis is related to hypercoagulable state and intrinsic small-vessel vasculopathy. The optimal management remains an unsolved problem and long-term anticoagulation have been recommended for cerebral ischemic events based on the presumed pathogenesis. There are controversial results in treatment of SS with immunomodulatory agents. We reported a case of a 49-year old women patient with recurrent ischemic cerebrovascular accidents as the first manifestation, accompanied by livedo reticularis in trunk and limbs and mitral valvulopathy without antiphospholipid antibody.
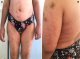
Figure 1: A) livedo reticularis in trunk and limbs; B) livedo reticularis in arms