Talar body fracture combined with medial malleolar fracture: a case report and literature review
Kamal Lahrach, Khalid Ibn El Kadi, Amine Marzouki, Fawzi Boutayeb
Corresponding author: Kamal Lahrach, Department of Orthopedic Surgery A, University Hospital Hassan II, Faculty of Medicine and Pharmacy, F�s, Morocco 
Received: 22 Jan 2015 - Accepted: 18 May 2015 - Published: 31 Jan 2019
Domain: Clinical medicine
Keywords: Talar body, medial malleolus, sagittal fracture, osteosynthesis
©Kamal Lahrach et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Kamal Lahrach et al. Talar body fracture combined with medial malleolar fracture: a case report and literature review. Pan African Medical Journal. 2019;32:57. [doi: 10.11604/pamj.2019.32.57.6166]
Available online at: https://www.panafrican-med-journal.com//content/article/32/57/full
Original article 
Talar body fracture combined with medial malleolar fracture: a case report and literature review
Talar body fracture combined with medial malleolar fracture: a case report and literature review
Kamal Lahrach1,&, Khalid Ibn El Kadi1, Amine Marzouki1, Fawzi Boutayeb1
1Department of Orthopedic Surgery A, University Hospital Hassan II, Faculty of Medicine and Pharmacy, Fès, Morocco
&Corresponding author
Kamal Lahrach, Department of Orthopedic Surgery A, University Hospital Hassan
II,
Faculty
of
Medicine and Pharmacy, Fès, Morocco
The incidence of talar fractures is lower (0.3%) and talar body fractures are the most frequent (60% of all talar fractures) [1]. A combination of a sagittal talar fracture and medial malleolar fracture seems to be very rare. Sporadic cases have been reported with unpredictable outcome, severe complications dominated by aseptic necrosis and osteoarthritis. However, association of medial malleolus fracture would preserve vascular branches from the deltoid ligament and irrigating the slope and therefore, limit the risk of necrosis. We discuss a case of this association in the literature review.
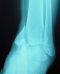
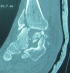
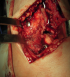
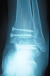
MKL, 52 year-old man, official, without medical history, was the victim of a traffic accident (motor vehicle accident) driving home blunt trauma of the right ankle with pain and overall functional impairment. The mechanism associated dorsiflexion, inversion and axial compression. Clinical examination revealed a large inflammatory ankle. The medial malleolus was very painful on palpation. There was no open wound, or neurovascular disorders. Radiographic and CT scan showed an ankle fracture oblique to the medial malleolus and a sagittal talar body fracture (Figure 1, Figure 2). A first reduction was performed by emergency maneuver the hard boot and abduction. The treatment consisted on surgery the next day under spinal anesthesia. Through the fracture of the medial malleolus, talus fracture was reduced and stabilized by two cancellous screws. Then the medial malleolus was reduced and fixed by two screws (two malleolar screws) (Figure 3). Contention by plaster boot was made for a period of six weeks. Postoperative radiological control was satisfactory (Figure 4). After removal of the boot, functional rehabilitation was established, and the vertical integration with full support was authorized for three months postoperatively. Six months after surgery, the patient shows no discomfort or pain, he gets back his work without any complaint (but 6 months is too short to eliminate osteonecrosis and osteoarthritis).
Fractures of the talus are rare (0.3% of all fractures), they are often associated with fractures of the neck of the foot, including a broken ankle in 26 % of cases [1-5]. The combination of a body sagittal fracture of the talus and the medial malleolus is exceptional. Few cases have been reported [4, 6-8]. Fractures of the talus follow an axial compression between the talus and the calcaneus tibiofibular mortise associated with forced dorsiflexion of the foot (5). This mechanism occurs when high-energy accidents: airplane crashes (rudder), car, motorcycle, fall from high altitude [3, 5, 9]. The existence of a medial malleolar fracture requires, in addition to the axial compression of the dorsiflexion a forced supply of the foot [5]. The bank then comes up against the mortise ceiling to superom�dial angle and it thus occurs concomitantly a vertical fracture of the talus and the medial malleolus [5, 6]. Thus lesions located on the medial side of the body of the talus require supination, so the lateral side of the lesions occurs in fractures with pronation and external rotation [10]. Each fracture of the talus described in our patient is classified C according to the classification of Sneppen et al. [10] and B according to the AO classification. But these classifications are incomplete, because they don't consider the associated malleolar fractures [6, 11]. Vascularization of the slope is precarious; it is influenced by three arteries: posterior tibial, anterior tibial and perforating branch of the peroneal artery. The medial half of the body of the talus is vascularized by the collateral of the posterior tibial artery from hich deltoid artery travels in the deltoid ligament [12]. The presence of an ankle fracture reduces the risk of developing post- traumatic necrosis of the talus preserving capsuloligamentary between the fragments of the talus and fractured malleolus [3, 4, 6, 13]. But the risk of post- traumatic necrosis depends also of soft tissue lesions, vascular damage, the force of trauma, and therapeutic quality [14, 15]. It occurs in 40 % of cases [10, 16]. Post-traumatic osteoarthritis is unpredictable; it is directly influenced by the importance of trauma and progressive complications [17]. Surgical treatment is required a. The reduction in open hearth articular surfaces must be complete and anatomical followed by internal fixation, is stable [14, 15, 18] by screwing or stay for the medial malleolus. The materials used are small screws or pins for slopes and cancellous screws or plug bracing for medial malleolus [18, 19]. The choice of incision is anteromedial, remote vascular pedicles [17]. The osteotomy of the medial malleolus, which is recommended to better expose the talus [20], is replaced by the fracture.
Fracture of the talus body is rare. The association with a medial malleolus fracture is exceptional, but providential infact it protects vasculature fragments detached and offers for one day an anatomic reconstruction of the talus. A support with rapid restoration of articular congruence and stable internal fixation can yield a good functional outcome.
The authors declare no competing interests.
All authors have contributed to this article and have read and agreed to the final manuscript.
Figure 1: radiography on admission
Figure 2: computed tomogram
on admission
Figure 3: intraoperative
photography shows before and after fixation screw
Figure 4: postoperative radiological control with a little fragment of fracture anterior to the body
- Court-Brown CM, Caesar B. Epidemiology of adult fractures: a review. Injury. 2006; 37(8):691-7. PubMed | Google Scholar
- Isaacs J, Courtenay B, Cooke A, Gupta M. Open reduction and internal fixation for concomittant talar neck, talar body, and medial malleolar fractures: a case report. J Orthop Surg Hong Kong. 2009; 17 (1):112-5. PubMed | Google Scholar
- Milenkovic S, Stanojkovic M. Hawkins type III fracture: dislocation of the talus and fracture of the medial malleolus treated by distraction external fixation. Unfallchirurg .2008; 111(2):112-6. PubMed | Google Scholar
- Montane I, Zych GA. An unusual fracture of the talus associated with a bimalleolar ankle fracture. A case report and review of the literature. Clin Orthop Relat Res .1986 jul; (208):278-81. PubMed | Google Scholar
- Hawkins LG. Fractures of the neck of the talus. J Bone Joint Surg Am. 1970; 52 (5):991-1002. PubMed | Google Scholar
- Verettas DA, Ververidis A, Drosos GI, Chatzipapas CN, Kazakos KI. Talar body fracture combined with bimalleolar fracture. Arch Orthop Trauma Surg .2008 jul;128 (7):731-4. PubMed | Google Scholar
- Saidi H, Ayach A, Fikry T. Fracture rare du corps du talus: � propos d'un cas et revue de litt�rature. Med Chir Pied. 2008;24(1):22-24. Google Scholar
- Kinkp� CVA, Dakour� PWH, Dansokho AV. Fracture du corps du talus associ�e � une fracture mall�olaire m�diale: � propos d'un cas bilat�ral. M�d Chir Pied. 2010 ; 26 (1):17-20. Google Scholar
- White SL, Harpaz NT, Jolly GP, Gorecki GA. High-energy bilateral talar neck fractures secondary to motocross injury. J Foot Ankle Surg. 1999; 38 (3):214-8. PubMed | Google Scholar
- Sneppen O, Christensen SB, Krogsoe O, Lorentzen J. Fracture of the body of the Talus. Acta Orthop Scand. 1977; 48(3): 317-24. PubMed | Google Scholar
- Devalia KL, Ismaiel AH, Joseph G, Jesry MG. Fourteen years follow up of an unclassified talar body fracture with review of literature. Foot and Ankle Surg. 2006; 12 (2):85-8. Google Scholar
- Haliburton RA, Sullivan CR, Kelly PJ, Peterson LF. The extra-osseous and intra-osseous blood supply of the talus. J Bone Joint Surg Am. 1958 Oct;40-A(5):1115-20. PubMed | Google Scholar
- Tehranzadeh J, Stuffman E, Ross SDK. Partial Hawkins sign in fractures of the talus: a report of three cases. AJR Am J Roentgenol. 2003; 181(6):1559-63. Google Scholar
- Curvale G, Bataille JF, Rochwerger A. Fractures et luxations du talus. Encycl Med Chir Appareil locomoteur. 1997;14(091):A-10.
- Baumhauer JF, Alvarez RG. Controversies in treating talus fractures. Orthop Clin North Am. 1995 Apr;26(2):335-51. PubMed | Google Scholar
- Higgins TF, Baumgaertner MR. Diagnosis and treatment of fractures of the talus: a comprehensive review of the literature. Foot Ankle Int. 1999 sep; 20(9): 595-605. PubMed | Google Scholar
- Trillat A, Bousquet G, Lapeyre B. Displaced fractures of the neck or of the body of the talus: alue of screwing by posterior surgical approach. Rev Chir Orthop. 1970;56(6):529-36. PubMed | Google Scholar
- Mendonca AD, Maury AC, Makwana NK. A simultaneous fracture of the tibia and talar body. Foot and Ankle Surg. 2004;10(1):45-7. Google Scholar
- Shah K, Hakmi A. Unusual ankle injury: a case report. The Foot. 2004;14(3):169-72. Google Scholar
- Adelaar RS. The treatment of complex fractures of the talus. Orthop Clin North Am. 1989 oct;20(4):691-707. PubMed | Google Scholar