Non alcoholic fatty liver disease in a young male with celiac disease
Zain Majid, Ghous Bux Somoro, Muhammad Manzoor ul Haque, Raja Taha Yaseen, Shoaib Ahmed Khan, Inamullah Khan Achakzai, Muhammad Ali Khalid, Nasir Hassan Luck
Corresponding author: Zain Majid, Department of Hepatogastroenterology, Sindh Institute of Urology and Transplantation (SIUT), Karachi, Pakistan 
Received: 15 Jun 2018 - Accepted: 25 Sep 2018 - Published: 16 Jan 2019
Domain: Gastroenterology
Keywords: Celiac disease, NASH, gluten free diet, BMI
©Zain Majid et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Zain Majid et al. Non alcoholic fatty liver disease in a young male with celiac disease. Pan African Medical Journal. 2019;32:25. [doi: 10.11604/pamj.2019.32.25.16345]
Available online at: https://www.panafrican-med-journal.com//content/article/32/25/full
Non alcoholic fatty liver disease in a young male with celiac disease
Zain Majid1,&, Ghous Bux Somoro1, Muhammad Manzoor Ul Haque1, Raja Taha Yaseen1, Shoaib Ahmed Khan1, Inamullah Khan Achakzai1, Muhammad Ali Khalid1, Nasir Hassan Luck1
1Department of Hepatogastroenterology, Sindh Institute of Urology and Transplantation (SIUT), Karachi, Pakistan
&Corresponding author
Zain Majid, Department of Hepatogastroenterology, Sindh Institute of Urology and Transplantation (SIUT), Karachi, Pakistan
A young emaciated male, known case of celiac disease came with the complains of diarrhea along with 5kgs of weight loss in 3 months' time. He had severe electrolyte abnormalities along with low albumin, low calcium and a high phosphate with deranged liver function test. Ultrasound abdomen had shown fatty liver. Nutrition consult was sought and he was found to have a BMI of 6.8kg/m2. He was started on nutrition support along with supportive therapy, which resulted in weight gain and improvement in his condition.
Celiac disease is an autoimmune disease characterized by gluten sensitivity, affecting genetically affected individuals [1]. It has intestinal and many extra intestinal features, while diagnosis requires both serological evidence along with small intestinal biopsy suggestive of the disease [1].
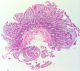
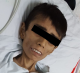
A 22-year-old emaciated male presented to the gastroenterology clinic of our department with the complains of diarrhea and weight loss since the last 3 months. His old record revealed him to be a diagnosed case of celiac disease, having been diagnosed 3 years prior to this admission, which was based upon his Tissue Transglutaminase serology (TTG serology) and duodenal biopsy report (Figure 1). He was later started on gluten free diet (GFD) and was initially compliant on it for a year. Later on, he became non-compliant and had been so ever since then. Currently his loose stools were watery in consistency, occurring 7-8 times per day. They were foul smelling, being difficult to flush, associated with tenesmus and with weight loss of around 5 kgs during this same time period. He did not complain of decrease in his appetite during this time nor had any history of fever, nausea, vomiting or of dysphagia. On examination, he appeared severely wasted with thin brittle hair along with dry skin and had prominent costal margins (Figure 2). His initial lab reports showed a low hemoglobin 10.2 g/dL along with a low platelet count 102,000 109fL. He was also found to have a severe electrolyte in-balance along with a low potassium (2.5 mEq/L), a low calcium (7.6 mg/dL), low albumin 1.8 g/dL, high phosphate 6.4 mg/dL and deranged LFTs with a TBR 0.48 U/L, ALP 303 U/L, SGPT 101 U/L, SGOT 65 U/L GGT 29 U/L. His iron profile, B12 and folate levels were sent along with lipid profile, which were all within normal limits. Ultrasound abdomen was later done and revealed diffuse fatty liver. His currently height was 132cm, while his weight was of 11.5kg along with a BMI 6.8 kg/m2. A nutritionist was immediately taken on board and he was started on blendized diet along with total parenteral nutrition and with replacement of his deranged electrolytes. His condition later improved within a week followed by weight gain of 3 kgs in one week. His oral intake gradually improved and his intravenous nutritional support was gradually tapered off. He regained 4 kg of weight and was later discussed and advised for regular follow-ups.
Many forms of hepatic diseases can be seen in those affected with celiac disease, including non alcoholic fatty liver disease and Nonalcoholic steatohepatitis (NASH) [2]. Non-alcoholic fatty liver disease or NAFLD is said to the commonest cause of chronic liver disease in the developed world [3, 4]. Celiac disease is seen in 4 to 13% in those having NASH [2]. The exact mechanism of this association is not known but it is plausible that this may be due to the increased intestinal permeability along with malabsorption of choline, a lipotropic factor and vitamin B6 [2]. According to one study, celiac disease is more often seen amongst those NAFLD patients having a BMI less than 27 kg/m2 [5]. This risk of NAFLD in celiac disease is mainly seen during the first year of life and does remain even after that [6]. It is said that GFD may help those celiac patients who have NAFLD, but the long term effects of this are still unknown [7].
Our case report suggests the importance of timely checking of LFTs in celiac disease patients, which could help prevent further complications in these patients.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: low-power
view showing moderate villous stunting and crypt hyperplasia,
consistent with Marsh class 3b (H&Ex40)
Figure 2: physical
appearance of the patient
- Gujral N, Freeman HJ, Thomson AB. Celiac disease: prevalence, diagnosis, pathogenesis and treatment. World J Gastroenterol. 2012 Nov 14; 18(42): 6036-59. PubMed | Google Scholar
- Kaushal K, Prasad, Uma Debi, Saroj K, Sinha, Chander K, Nain, Kartar Singh. "Hepatobiliary Disorders in Celiac Disease: an update." International Journal of Hepatology. 2011; 2011: 438184. PubMed | Google Scholar
- Dyson JK, Anstee QM, McPherson S. Non-alcoholic fatty liver disease: a practical approach to treatment. Frontline Gastroenterology. 2014; 5(4): 277-286. PubMed | Google Scholar
- Tasneem AA, Luck NH, Majid Z. Factors predicting non-alcoholic steatohepatitis (NASH) and advanced fibrosis in patients with non-alcoholic fatty liver disease (NAFLD). Trop Doct. 2018 Apr; 48(2): 107-112. PubMed | Google Scholar
- Anania C, De Luca E, De Castro G, Chiesa C, Pacifico L. Liver involvement in pediatric celiac disease. World J Gastroenterol. 2015 May 21; 21(19): 5813-22. PubMed | Google Scholar
- Reilly NR, Lebwohl B, Hultcrantz R, Green PH, Ludvigsson JF. Increased risk of non-alcoholic fatty liver disease after diagnosis of celiac disease. J Hepatol. 2015 Jun; 62(6): 1405-11. PubMed | Google Scholar
- Rubio-Tapia A, Murray JA. Liver involvement in celiac disease. Minerva Med. 2008 Dec; 99(6): 595-604. PubMed | Google Scholar