Genetic diversity of Plasmodium falciparum infection among children with uncomplicated malaria living in Pointe-Noire, Republic of Congo
Pembet Singana Brice, Pembe Issamou Mayengue, Niama Roch Fabien, Ndounga Mathieu
Corresponding author: Pembe Issamou Mayengue, Facult� des Sciences et Techniques, Universit� Marien Ngouabi, BP 69 Brazzaville, R�publique du Congo, Laboratoire National de Sant� Publique, BP 120 Brazzaville, R�publique du Congo 
Received: 04 Apr 2018 - Accepted: 12 Dec 2018 - Published: 12 Apr 2019
Domain: Epidemiology,Molecular Biology,Parasitology
Keywords: Plasmodium falciparum, genetic diversity, multiplicity of infection, msp-1, msp-2, Republic of Congo
©Pembet Singana Brice et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Pembet Singana Brice et al. Genetic diversity of Plasmodium falciparum infection among children with uncomplicated malaria living in Pointe-Noire, Republic of Congo. Pan African Medical Journal. 2019;32:183. [doi: 10.11604/pamj.2019.32.183.15694]
Available online at: https://www.panafrican-med-journal.com//content/article/32/183/full
Original article 
Genetic diversity of Plasmodium falciparum infection among children with uncomplicated malaria living in Pointe-Noire, Republic of Congo
Genetic diversity of Plasmodium falciparum infection among children with uncomplicated malaria living in Pointe-Noire, Republic of Congo
Brice Pembet Singana1, Pembe Issamou Mayengue1,2,&, Roch Fabien Niama1,2, Mathieu Ndounga3
1Facult� des Sciences et Techniques, Universit� Marien Ngouabi, BP 69 Brazzaville, R�publique du Congo, 2Laboratoire National de Sant� Publique, BP 120 Brazzaville, R�publique du Congo, 3Programme National de Lutte contre le Paludisme, Direction G�n�rale de l�Epid�miologie de la Maladie, Minist�re de la Sant� et de la Population, R�publique du Congo
&Corresponding author
Pembe Issamou Mayengue, Facult� des Sciences et Techniques, Universit� Marien Ngouabi, BP 69 Brazzaville, R�publique du Congo, Laboratoire National de Sant� Publique, BP 120 Brazzaville, R�publique du Congo
Introduction: molecular characterization of malaria parasites from different localities is important to improve understanding of acquisition of natural immunity to Plasmodium falciparum, to assist in identifying the most appropriate strategies for control and to evaluate the impact of control interventions. This study aimed to determine the genetic diversity and the multiplicity of infection in Plasmodium falciparum isolates from Pointe-Noire, Republic of Congo.
Methods: Plasmodium falciparum isolates were collected from 71 children with uncomplicated malaria; enrolled into the study for evaluating the therapeutic efficacy of artemether-lumefantrine combination. Both msp-1 and msp-2 genes were genotyped.
Results: from 296 distinct fragments detected, 13 msp-1 and 27 msp-2 different alleles were identified. For msp-1, RO33 family was poorly polymorphic. The K1 family has shown the trend of predominance (41%), followed by Mad20 (35%). Comparatively to msp-2, 49.6% and 48.8% fragments belonged to 3D7 and FC27 respectively. Taking together msp-1 and msp-2 genes, the overall multiplicity of infection has been increased to 2.64 and 86% harbored more than one parasite genotype. Parasite density was not influenced by age as well as the multiplicity of infection which was not influenced neither by age nor by parasite density.
Conclusion: genetic diversity of Plasmodium falciparum in isolates from patients with uncomplicated malaria in Pointe-Noire is high and consisted mainly of multiple clones. The overall multiplicity of infection has been largely increased when considering msp-1 and msp-2 genes together. With the changes in malaria epidemiology, the use of both msp-1 and msp-2 genes in the characterization of Plasmodium falciparum infection is recommended.
Malaria, a disease mainly caused by Plasmodium falciparum, remains a public health concern. Although massive interventions deployed in sub-Saharan Africa have reduced the global malaria morbidity and mortality at 212 million and 429,000 deaths respectively in 2015, some sub-Saharan Africa region had provided partial data regarding the impact of certain interventions [1]. In the Republic of Congo, malaria is still the leading cause of attendance in health facilities. The latest estimations from the National Malaria Control Program indicate that clinical malaria account for 47.9% of all outpatient consultations in public hospitals, 64.8% of hospital admissions and 18.4% of deaths [2]. The high levels of resistance of Plasmodium falciparum to chloroquine as well as the inefficacy of sulphadoxine-pyrimethamine and amodiaquine either singly or in combination for the treatment of uncomplicated malaria have been well documented [3-6]. Thus, the Republic of Congo has changed its anti-malarial drug policy for treating uncomplicated malaria to artemisinin-combination therapies (ACTs) in 2006 [7]. Studies aiming to evaluate the efficacy of these combinations have been conducted mainly in Brazzaville [8-10]. Only one was done in Owando, located in the north part of the Republic of Congo [11]. Although the efficacy of artesunate-amodiaquine and artemether-lumefantrine is still high as reported in these previous studies, it is important to extend the efficacy assessment as well as to evaluate the impact of these combinations on the malaria parasite population dynamic and the multiplicity of Plasmodium falciparum infection (MOI) in other localities, nine years after the implementation of artesunate-amodiaquine and artemether-lumefantrine in Republic of Congo.
�
Genetic diversity of circulating Plasmodium falciparum strain, the occurrence of variant forms of the parasite in different geographic areas and variation of MOI after recombination between genetically distinct gametocytes, constitute the major obstacles to the design of a malaria vaccine [12, 13]. Consequently, these two parameters allow characterization of malaria parasites in human populations and improve understanding of acquisition of natural immunity to Plasmodium falciparum and would assist in identifying the most appropriate strategies for control and also to evaluate the impact of control interventions [14, 15]. The merozoite surface protein-1 (msp-1) and merozoite surface protein-2 (msp-2) are asexual blood stage antigens that are considered prime candidates for the development of malaria vaccine, and also suitable markers used extensively to identify genetically distinct Plasmodium falciparum parasite sub-populations in many malaria endemic countries as well as to distinguish recrudescence to re-infection in anti-malarial drug trials and efficacy [16-18]. It has been proposed that with the change of malaria epidemiology, both msp-1 and msp-2 allele frequency and genetic diversity should be monitored regularly to ensure the reliability of the PCR (polymerase chain reaction)-adjusted treatment outcome [18]. To our knowledge, in the Republic of Congo, after the introduction of artemisinin combination therapy (ACTs), the most epidemiological studies on Plasmodium falciparum genetic diversity have been conducted in Brazzaville [15, 19]. However, only one has been done in one health facility in the city of Pointe-Noire, the second largest city in the country, using msp-2 gene as marker [20]. Conversely, there is no information on msp-1 diversity in Pointe-Noire. During the study aiming the efficacy assessment of artemether-lumefantrine combination in Pointe-Noire in 2015, we proposed to determine the genetic diversity of Plasmodium falciparum in the recruited population using both msp-1 and msp-2 markers.
Study area
�
The present study was conducted at the �Centre de Sant� Int�gr� de Mbota� located in the eastern part of the city of Pointe-Noire, the economic capital of the Republic of Congo, separated by 510km from Brazzaville. Two rainy seasons are observed each year with the main one during the months of February to May, and a short one from October to December. Malaria endemicity is high with perennial transmission and peaks during the rainy season, which normally runs from October to May [3] and malaria infection is primarily due to Plasmodium falciparum.�
Study population and blood samples collection�
Infected blood with Plasmodium falciparum was collected from children under 13 years old enrolled into the study (study ACTRN12615001110572) for evaluating the therapeutic efficacy of artemether-lumefantrine combination from September to November 2015. Diagnostic of Plasmodium falciparum was confirmed by light microscopy on thick blood smears. Malaria parasites were quantified against 200 leucocytes. Parasite density was calculated for each patient assuming an average of 8,000 leucocytes per �L of blood using the proposed method of the WHO [21]. Before treatment, blood sample from each patient was blotted on the Watman filter paper (3MM CHR), dried and transferred to the �Laboratoire National de Sant� Publique� in Brazzaville, where isolation of DNA and genotyping were performed. The clinical study on artemether-lumefantrine efficacy was approved by the institutional �Comit� d�Ethique de la Recherche en Sciences de la Sant� (N� 038/DGRST/CERSSA in June 2015) of the Congolese Ministry of Research and the Ministry of Health and Population of Republic of Congo.�
Extraction of parasite DNA�
Genomic DNA was extracted from samples collected on the Watman filter paper by QIAamp DNA mini Kit (Qiagen, Hilden, Germany) according to the manufacturer�s instruction. Extracted DNA was stored at -20�C until use.�
Plasmodium falciparum msp-1 and msp-2 genotyping�
Samples genotyping of Plasmodium falciparum was performed using the nested polymerase chain reactions (PCRs) technique. The merozoite surface protein-1 (msp-1) and merozoite surface protein-2 (msp-2) genes in their highly polymorphic loci, namely msp-1 block 2 and msp-2 central region were used as markers for this genotyping as described previously [16, 17, 22, 23]. PCR amplification was performed following a 2-step amplification procedure, in which the initial amplifications were followed by individual nested PCR reactions using specific primers for K1, Mad20 and RO33 allelic families for msp-1, and FC27 and 3D7 allelic families for msp-2 (Table 1). Allelic specific and DNA free negative controls were included in each step of the reaction. Five microliters of each of the PCR products were loaded on 2% agarose gel (PeqLab, Erlangen, Germany), stained with ethidium bromide, separated by electrophoresis and visualized under ultraviolet trans-illumination. Individual alleles were identified by fragment length and by the corresponding allele-specific primers used and the size of the PCR products were estimated using 100bp DNA ladder marker (Invitrogen, Karlsruhe, Germany). The size polymorphism in each allelic family (Table 1), assuming that one band represented one amplified PCR fragment derived from a single copy of Plasmodium falciparum msp-1 and msp-2 genes. Alleles in each family were considered the same fragment size was within 20 bp interval [17].�
Data and statistical analysis�
The frequency of msp-1 and msp-2 allele was calculated as the proportion of allele found for the allelic family out of the alleles detected in isolates. The mean expected heterozygosity (He) value for each allelic family of msp-1 and msp-2 genes was calculated as described by Mohd Abd Razak et al. [24]. The detection of one msp-1 and msp-2 allele was considered as one parasite genotype. The multiplicity of infection was defined as the minimum number of Plasmodium falciparum genotypes per infected subject and estimated by dividing the number of amplified PCR fragments reflecting the parasite genotypes by the number of positive samples. Chi-square test was applied to compare proportions. Spearman�s rank correlation coefficients were calculated to assess association between multiplicity of infection (MOI) and geometric mean parasite density and age. Differences were considered significant if P values < 0.05.
Characteristics of patients and parasite density
�
A total of 71 patients with malaria and microscopically confirmed Plasmodium falciparum only were enrolled in the study, with 34 (47.9%) and 37 (52.1%) being males and females respectively. Twenty-six and 45 were children aged between 1 to 4 years old and 5 to 12 years old respectively. The geometric mean parasite density was 36,699.6 parasites/�l of blood with the range of 1,435-349,700 parasites/�l (Table 2).�
Plasmodium falciparum genotyping of msp-1 and msp-2�
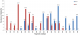
All 71 samples were analyzed for polymorphisms on msp-1 and msp-2 genes. The efficiency of msp-1 and msp-2 genes amplification reactions with family-specific primers were 100% and 97.2% respectively. With a total of 296 distinct fragments detected, 13 msp-1 and 27 msp-2 different alleles were identified. The msp-1 gene analysis showed 70, 60, 41 fragments belonged to K1 (41% of overall detected msp-1 alleles), Mad20 (35%) and R033 (24%) families respectively. Eight K1 type alleles (He value of 0.82), 4 Mad20 (He value of 0.68) type alleles and only 1 RO33 type allele (150 pb) were identified, with no statistical significant predominance of any specific family (Figure 1). The msp-2 gene yielded 13 3D7 type alleles (He value of 0.92) and 14 FC27 type alleles (He value of 0.93), with no statistical significant predominance of any specific family (Figure 2). Out of 123 fragments identified, 62 fragments belonged to 3D7 (49.6% of overall detected msp-2 alleles) and 61 belonged to FC27 (48.8%). Two genotypes (1.6%) could not be assigned to any specific family.�
Plasmodium falciparum multiplicity of infections, parasite densities in relation to age�
When considering msp-1 and msp-2 genes separately, the MOI was 2.40 and 1.74 respectively, while 55 (77.46%) and 34 (47.88%) of isolates contained multiclonal infection at least with 2 clones respectively. Taking together msp-1 and msp-2 genes, the overall MOI was 2.64 and 61 (86%) isolates harbored more than one parasite genotype. No statistical significant difference was observed in the MOI between patients with less than 5 years old (2.44) and those with the age between 5 and 12 years old (2.40) with the p-value = 0.972. The combinations of msp-1 and msp-2 different parasite genotypes were not associated with the parasite density (Table 3), as well as the MOI was not associated with parasite density (Table 4). Moreover, the age was not associated significantly with the parasite density (p-value = 0.381). Taking together, no statistical significant difference was observed in the parasite densities and the MOI according to the age (Figure 3).
The genetic diversity may be an important element for implementing malaria control strategies in the country, as elimination may influence genetic diversity [25]. In the Republic of Congo, most of the studies on the Plasmodium falciparum genetic diversity using merozoite surface protein genes which are considered like robust and suitable markers [22, 25, 26] have been conducted in Brazzaville, the political capital [5, 15, 17, 19, 27]. With the expanding access to ACT and current changes in malaria epidemiology, it has been encouraged to monitor regularly the Plasmodium falciparum msp-1 and msp-2 allele frequency-genetic diversity [18], despite some debate around their usefulness as markers of population structure [14, 28]. To our knowledge, this present study represents the first investigation of genetic diversity of Plasmodium falciparum populations to employ both msp-1 and msp-2 gene markers, 9 years after the implementation of ACTs for the treatment of uncomplicated Plasmodium falciparum malaria in Pointe-Noire.
�
Allelic specific PCR typing of msp-1 and msp-2 genes showed a high genetic diversity in the Plasmodium falciparum population in the analyzed isolates. The degree of polymorphism found in the present study is also consistent with the previous findings in the same area using microsatellites markers [29]. The msp-2 gene has showed a high diversity as previously reported in Pointe-Noire [20]. Although msp-1 gene was amplified in all isolates, genetic diversity still low compared to msp-2 gene as previously described in the country [17]. With regard to msp-1, the presence of Mad20, K1 and R033 allelic families in the 71 isolates was noticed. RO33 family was poorly polymorphic with only one allele as reported in previous studies in Brazzaville and other countries such as Senegal, Iran, Nigeria and Brazil [13, 17, 30-32] in contrast to findings in Gabon and C�te d�Ivoire [33]. Although the K1 family has shown the trend of predominance (41%), followed by Mad20 (35%), the difference in prevalence between these free families was not statistically significant. Comparatively to msp-2, no predominance to any allelic family was found. Taking together msp-1 and msp-2, our findings are in contrast to those reported in previous studies in Brazzaville and other countries such as Gabon, Benin, Ghana, and Ethiopia where K1 for msp-1 and 3D7 for msp-2 were predominantly found in isolates from uncomplicated malaria [17, 25, 33-36].�
The trend observed in the prevalence of K1 and 3D7 families in the current study may be related to the limited sample size. Repeated studies including a large sample size and different sites including symptomatic and asymptomatic Plasmodium falciparum infection in Pointe-Noire are needed to better characterize the allelic polymorphism of Plasmodium falciparum in this city. Understanding the diversity of Plasmodium falciparum has implications for vaccine since the major obstacles to the design of an efficient malaria vaccine is the large genetic diversity of vaccine targets allowing parasites with mutated genes to escape from the host�s immune response [16]. Thus, different genetic profiles of malaria parasites even within or between countries should be taken into account in the prospect of vaccine development against Plasmodium falciparum for improving vaccine design.�
The presence of more than one parasite genotype was detected in 86% of isolates from Pointe-Noire, with the MOI values for msp-1 and msp-2 genes of 2.40 and 1.74 respectively. The overall MOI value of 2.64 was found, when taking together msp-1 and msp-2 genes and this was higher than values obtained from Brazzaville, even before or after the introduction of ACTs [5, 17, 19, 20]. Despite the lack of entomological data from Pointe-Noire and Brazzaville, the number of clones coinfecting a single host can be used as an indicator of the level of malaria transmission or the level of host acquired immunity [12, 28, 33, 37]. Therefore, the discrepancies on the MOI may suggest the different level of malaria transmission between these two cities, with Brazzaville being more urbanized. Studies conducted in Mali and Malawi have confirmed lowest levels of MOI and proportions of polygenomic infections in areas exhibiting low malaria transmission, namely in the urban sites and highest levels where malaria transmission is almost perennial [38, 39]. Multiple parasite types in a single human host have been suggested to lead to cross fertilization, meiotic recombination and generation of new strains during the developmental stage in the mosquito [12, 13, 40]. This supports the fact that both MOI and polymorphism are high in Pointe-Noire. Since no data are available on the MOI in Pointe-Noire before the introduction of ACT, it seems difficult to evaluate the impact of this measure on the MOI in this city. The MOI was influenced neither by age nor by parasite density in this population in contrast with the previous findings in Brazzaville, Tanzania and Sudan [17, 26, 41, 42], but concordant with those in Ethiopia and Mali [25, 39]. Therefore, regardless of the parasite densities, and the fact that the samples collection has been done during the peak malaria transmission, the prevalence of multi clonal infections affected all the two age groups.
Genetic diversity of Plasmodium falciparum in isolates from patients with uncomplicated malaria in Pointe-Noire, Republic of Congo is high and consisted mainly of multiple clones. By considering msp-1 and msp-2 genes together, the overall multiplicity of infection has been largely increased. Thus, with the changes in malaria epidemiology, this study supports the use of both msp-1 and msp-2 genes in the characterization of Plasmodium falciparum infection, when the MOI is considered like one of the major parameters to be evaluated for malaria control interventions.
What is known about this topic
- Malaria is still the leading cause of attendance in health facilities in many sub-Saharan countries;
- Plasmodium falciparum genetic diversity would assist in identifying the most appropriate strategies for control and also to evaluate the impact of control interventions as well as changes in malaria epidemiology;
- Little data available regarding the Plasmodium falciparum genetic diversity and the MOI using both msp-1 and msp-2 as molecular markers, particularly in Pointe-Noire, the Republic of Congo.
What this study adds
- Genetic diversity of Plasmodium falciparum is high and consisted mainly of multiple clones in Pointe-Noire;
- Increase MOI when msp-1 and msp-2 are used together as molecular markers;
- The epidemiological trend of malaria seems to be different between Pointe-Noire and Brazzaville in the Republic of Congo.
The authors declare no competing interests.
NM designed and coordinated field study. NM and PSB conducted enrollment, patients follow-up, field samples and data collection; PSB and PIM processed the samples and analyzed the data; PSM, PIM, NRF, and NM wrote the draft paper. All authors read and approved the final version and the final manuscript.
We are grateful to all patients and parents who participated in this study. Enrollment of patients and samples collection was founded by Bill and Melinda Gates Foundation (Grant N� 51936) through WHO. Molecular genotyping has been done and funded by the �Laboratoire National de Sant� Publique�, Republic of Congo. We are grateful Professor Henri Joseph Parra for making facilities available for this study.
Table 1: oligonucleotides sequences used for single and nested polymerase chain reaction (PCR) of Plasmodium falciparum msp-1 and msp-2 genes [16] and range of fragment size of the alleles
Table 2: characteristics of patients with uncomplicated Plasmodium falciparum malaria in Pointe- Noire, Republic of Congo
Table 3: distribution of msp-1 and msp-2 detected allelic families according to the parasite densities
Table 4: profile of multiple infections according to the parasite densities
Figure 1: prevalence of Plasmodium falciparum msp-1 alleles in clinical isolates from Pointe-Noire, Republic of Congo
Figure 2: prevalence of Plasmodium falciparum msp-2 alleles in clinical isolates from Pointe-Noire, Republic of Congo
Figure 3: relation between mean geometric density and multiplicity of infection with age
- WHO report. World malaria report. Geneva: World Health Organization, 2016. Accessed December 13, 2016.
- Koukouikila-Koussounda F, Ntoumi F. Malaria epidemiological research in the Republic of Congo. Malar J. 2016;15(1):598. PubMed | Google Scholar
- Nsimba B, Malonga DA, Mouata AM, Louya F, Kiori J, Malanda M et al. Efficacy of Sulfadoxine/pyrim�thamine in the treatment of uncomplicated Plasmodium falciparum malaria in Republic of Congo. Am J Trop Med Hyg. 2004; 70(2):133-138. PubMed | Google Scholar
- Nsimba B, Jafari-Guemouri, Malonga DA, Mouata AM, Kiori J, Louya F et al. Epidemiology of drug-resistant malaria in Republic of Congo: using molecular evidence for monitoring antimalarial drug resistance combined with assessment of antimalarial drug use. Trop Med Int Health. 2005; 10(10):1030-1037. PubMed | Google Scholar
- Mayengue PI, Ndounga M, Davy MM, Tandou N, Ntoumi F. In vivo chloroquine resistance and prevalence of the pfcrt codon 76 mutation in Plasmodium falciparum isolates from the Republic of Congo. Acta Trop. 2005; 95(5):219-225. PubMed | Google Scholar
- Ndounga M, Mayengue PI, Tahar R, Casimiro PN, Matondo Maya DW, Miakassissa-Mpassi V et al. Efficacy of sulfadoxine-pyrimethemine, amodiaquine, and sulfadoxine-pyrimethamine-amodiaquine combination for the treatment of uncomplicated falciparum malaria in urban and surban areas of Brazzaville (Congo). Acta Trop. 2007; 103(3):163-171. PubMed | Google Scholar
- Ministry of Health and Population. Politique nationale de lutte contre le paludisme. Minist�re de la Sant� et de la Population, Brazzaville, R�publique du Congo. 2006. Consult� le 04 Avril 2017.
- Ndounga M, Tahar R, Casimiro PN, Loumouamou D, Basco LK. Clinical efficacy of artemether lumefantrine in Congolese children with acute uncomplicated falciparum malaria in Brazzaville. Malar Res Treat. 2012;2012:749479. PubMed | Google Scholar
- Ndounga M, Mayengue PI, Casimiro PN, Loumouamou D, Basco LK, Ntoumi F et al. Artesunate-amodiaquine efficacy in Congolese children with acute uncomplicated falciparum malaria in Brazzaville. Malar J. 2013; 12:53. PubMed | Google Scholar
- Ndounga M, Mayengue PI, Casimiro PN, Koukouikila-Koussounda F, Bitemo M, Matondo DB et al. Artesunate-amodiaquine versus artemether-lumefantrine for the treatment of acute uncomplicated malaria in Congolese children under 10 years old living in suburban area: a randomized study. Malar J. 2015; 14:423. PubMed | Google Scholar
- Singana BP, Bogreau H, Matondo BD, Dossou-Yovo LR, Casimiro PN, Mbouka R et al. Malaria burden and anti-malarial drug efficacy in Owando, northern Congo. Malar J. 2016; 15:16. PubMed | Google Scholar
- Akhouri RR, Bhattacharyya A, Pattnaik P, Malhotra P, Sharma A. Structural and functional dissection of the adhesive domains of Plasmodium falciparum thrombospondin-related anonymous protein (TRAP). Biochem J. 2004; 379(Pt 3):815-822. PubMed | Google Scholar
- Heidari A, Keshavarz H, Rokni MB, Jelinek T. Genetic diversity in merozoite surface protein (MSP)-1 and MSP-2 genes of Plasmodium falciparum in a major endemic region of Iran. Korean J Parasitol. 2007; 45(1):59-63. PubMed | Google Scholar
- Conway DJ, Cavanagh DR, Tanabe K, Roper C, Mikes ZS, Sakihama N et al. A principal target of human immunity to malaria identified by molecular population genetic and immunological analyses. Nat Med. 2000;6(6):689-92. PubMed | Google Scholar
- Ibara-Okabande R, Koukouikila-Koussounda F, Ndounga M, Vouvoungui J, Malonga V, Casimiro PN et al. Reduction of multiplicity of infections but no changes in msp2 genetic diversity in Plasmodium falciparum isolates from Congolese children after introduction of artemisinin-combination therapy. Malar J. 2012;11:410. Google Scholar
- Ntoumi F, Ngoundou-Landji J, Lekoulou F, Luty A, Deloron P, Ringwarld P. Site-base study on polymorphism of Plasmodium falciparum MSP-1 et MSP-2 genes in isolates from two villages in Central Africa. Parasitologia. 2000;42(3-4):197-203. Google Scholar
- Mayengue PI, Ndounga M, Malonga FV, Bitemo M, Ntoumi F. Genetic polymorphism of m�rozo�te surface protein-1 and merozoite surface protein-2 in Plasmodium falciparum isolates from Brazzaville, Republic of Congo. Malar J. 2011; 10:276. PubMed | Google Scholar
- Mwingira F, Nkwengulila G, Schoepflin S, Sumari D, Hans-Peter Beck, Snounou G et al. Plasmodium falciparum msp1, msp2 and glurp allele frequency and diversity in sub-Saharan Africa. Malar J. 2011;10:79. PubMed | Google Scholar
- Etoka-Beka MK, Ntoumi F, Kombo M, Deibert J, Poulain P, Vouvoungui C et al. Plasmodium falciparum infection in febrile Congolese children: prevalence of clinical malaria 10 years after introduction of artemisinin-combination therapies. Trop Med Int Health. 2016;21(12):1496-1503. PubMed | Google Scholar
- Ntoumi F, Vouvoungui JC, Ibara R, Landry M, Sidib� A. Malaria burden and case management in the Republic of Congo: limited use and application of rapid diagnostic tests results. BMC Public Health. 2013; 13:135. PubMed | Google Scholar
- World Health Organization. Parasitologie m�dicale: techniques de base pour le laboratoire. Genève, OMS. 1993
- Ekala MT, Jouin H, Lekoulou F, Issifou S, Mercereau-Puijalon O, Ntoumi F. Plasmodium falciparum merozoite surface protein 1 (MSP-1): genotyping and humoral responses to allele-specific variants. Acta trop. 2002;81(1):33-46. Google Scholar
- Mayengue PI, Luty AJ, Rogier C, Baragatti M, Kremsner PG, Ntoumi F. The multiplicity of Plasmodium falciparum infections is associated with acquired immunity to asexual blood stage antigens. Microbes Infect. 2009;11(1):108-114. PubMed | Google Scholar
- Mohd Abd Razak MR, Sastu UR, Norahmad NA, Abdul-Karim A, Muhammed A, Muniandy PK et al. Genetic diversity of Plasmodium falciparum populations in malaria declining areas of Sabah, East Malaysia. PLos One. 2016;11(3):e0152415. PubMed | Google Scholar
- Mohammed H, Mindaye T, Belayneh M, Kassa M, Assefa A, Tadesse M et al. Genetic diversity of Plasmodium falciparum isolates based on MSP-1 and MSP-2 genes from Kolla-Shele area, Arbaminch Zuria District, southwest Ethiopia. Malar J. 2015; 14:73. PubMed | Google Scholar
- Felger I, Tavul L, Kabintik S, Marshall V, Genton B, Alpers M et al. Plasmodium falciparum: extensive polymorphism in merozoite surface antigen 2 alleles in an area with endemic malaria in Papua New Guinea. Exp Parasitol. 1994;79(2):106-116. PubMed | Google Scholar
- Koukouikila-Koussounda F, Malonga V, Mayengue PI, Ndounga M, Vouvoungui CJ, Ntoumi F. Genetic polymorphism of merozoite surface protein 2 and prevalence of K76T pfcrt mutation in Plasmodium falciparum field isolates from Congolese children with asymptomatic infections. Malar J. 2012; 11:105. PubMed | Google Scholar
- Anderson TJ, Su XZ, Roddam A, Day PK. Complex mutations in a high proportion of microsatellite loci from the protozoan parasite Plasmodium falciparum. Mol Ecol. 2000; 9(10):1599-1608. PubMed | Google Scholar
- Durand P, Michalakis Y, Cestier S, Oury B, Leclerc MC, Tibayrenc M et al. Significant linkage disequilibrium and high genetic diversity in a population of Plasmodium falciparum from an area (Republic of the Congo) highly endemic for malaria. Am J Trop Med Hyg. 2003;68(3):345-349. PubMed | Google Scholar
- Zwetyenga J, Rogier C, Tall A, Fontenille D, Snounou G, Trape JF et al. No influence of age on infection complexity allelic distribution in Plasmodium falciparum infection in Ndiop, a Senegales village with seasonal, mesoendemic malaria. Am J Trop Med Hyg. 1998;59(5):726-35. PubMed | Google Scholar
- Sallenave-Sales S, Daubersies P, Mercereau-Puijalon O, Rahimalala L, Contamin H, Druilhe P et al. Plasmodium falciparum: a comparative analysis of the genetic diversity in malaria mesoendemic areas of Brazil and Madagascar. Parasitol Res. 2000;86(8):692-698. PubMed | Google Scholar
- Kolawole OM, Mokuolu OA, Olukosi YA, Oloyede TO. Population genomics diversity of Plasmodium falciparum in malaria patients attending Okelele Health Centre, Okelele, Ilorin, Kwara State, Nigeria. Afr Health Sci. 2016;16(3):704-711. PubMed | Google Scholar
- Yavo W, Konat� A, Mawili-Mboumba DP, Kassi KF, Mbuyi TML, Angora EK et al. Genetic Polymorphism of msp1 and msp2 in Plasmodium falciparum isolates from C�te d�Ivoire versus Gabon. J Parasitol Res. 2016; 2016:3074803. PubMed | Google Scholar
- Aubouy A, Migot-Nabias F, Deloron P. Polymorphism in two merozoite surface proteins of Plasmodium falciparum isolates from Gabon. Malar J. 2003; 2:12. PubMed | Google Scholar
- Kobbe R, Neuhoff R, Marks F, Adjei S, Langefeld I, von Reden C et al. Seasonal variation and higly multiplicity of first Plasmodium falciparum infections in children from a holoendemic area in Ghana, West Africa. Trop Med Int Health. 2006;11(5):613-619. Google Scholar
- Ogouy�mi-Hounto A, Gazard DK, Ndam N, Topanou E, Garba O, Elegbe P et al. Genetic polymorphism of merozoite surface protein-1 and merozoite surface protein-2 in Plasmodium falciparum isolates from children in South of Benin. Parasite. 2013;20:37. PubMed | Google Scholar
- Smith T, Felger I, Beck HP, Tanner M. Consequences of multiple infection with Plasmodium falciparum in an area of high endemicity. Parassitologia. 1999;41(1-3):247-250. PubMed | Google Scholar
- Bruce MC, Macheso A, McConnachie A, Molyneux ME. Comparative population structure of Plasmodium malariae and Plasmodium falciparum under different transmission settings in Malawi. Malar J. 2011;10:38. PubMed | Google Scholar
- Nabet C, Doumbo S, Jeddi F, Konat� S, Manciulli T, Fofana B et al. Genetic diversity of Plasmodium falciparum in human malaria cases in Mali. Malar J. 2016;15:353. PubMed | Google Scholar
- Snounou G, Zhu X, Siripoon N, Jarra W, Thaithong S, Brown KN et al. Biased distribution of mspl and msp2 allelic variants in Plasmodium falciparum populations in Thailand. Trans R Soc Trop Med Hyg. 1999;93(4):369-374. PubMed | Google Scholar
- Hamid MAM, Elamin AF, Albsheer MM, Abdalla AA, Mahgoub NS, Mustafa SO et al. Multiplicity of infection and genetic diversity of Plasmodium falciparum isolates from patients with uncomplicated and severe malaria in Gezira State, Sudan. Parasit Vectors. 2016;9(1):362. Google Scholar
- Kidima W, Nkwengulila G. Plasmodium falciparum msp2 Genotypes and multiplicity of infections among children under five years with uncomplicated Malaria in Kibaha, Tanzania. J Parasitol Res. 2015;2015:721201. PubMed | Google Scholar