Tuberculous lymphadenitis associated thrombocytopenic purpura, effectiveness of anti-tuberculous therapy
Nabil Ali Barrow, Jamilah Atallah Alatawi, Abid Saeed, Tariq Ali Alblowy, Hyder Osman Mirghani, Ayman Fisal Ahmed Foad
Corresponding author: Hyder Osman Mirghai, Department of Internal Medicine, Faculty of Medicine, University of Tabuk, Tabuk, Saudi Arabia 
Received: 03 Mar 2017 - Accepted: 25 Jun 2017 - Published: 15 Feb 2018
Domain: Haematology,Microbiology
Keywords: Immune thrombocytopenia, tuberculosis, Saudi Arabia
©Nabil Ali Barrow et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Nabil Ali Barrow et al. Tuberculous lymphadenitis associated thrombocytopenic purpura, effectiveness of anti-tuberculous therapy. Pan African Medical Journal. 2018;29:118. [doi: 10.11604/pamj.2018.29.118.12145]
Available online at: https://www.panafrican-med-journal.com//content/article/29/118/full
Original article 
Tuberculous lymphadenitis associated thrombocytopenic purpura, effectiveness of anti-tuberculous therapy
Tuberculous lymphadenitis associated thrombocytopenic purpura, effectiveness of anti-tuberculous therapy
Nabil Ali Barrow1, Jamilah Atallah Alatawi2, Abid Saeed3, Tariq Ali Alblowy4, Hyder Osman Mirghani5,&, Ayman Fisal Ahmed Foad6
1Clinical Haematology consultant, King Khalid Hospital, Tabuk, Saudi Arabia, 2Medical Intern, King Khalid Hospital, Tabuk, Saudi Arabia, 3Histopathology Specialist, King Khalid Hospital, Tabuk, Saudi Arabia, 4King Khalid Hospital, Tabuk, Saudi Arabia, 5Department of Internal Medicine, Faculty of Medicine, University of Tabuk, Tabuk, Saudi Arabia, 6Department of Pathology, Faculty of Medicine, University of Tabuk, Saudi Arabia
&Corresponding author
Hyder Osman Mirghai, Department of Internal Medicine, Faculty of Medicine, University of Tabuk, Tabuk, Saudi Arabia
The association of immune thrombocytopenic purpura and tuberculosis is extremely rare. We presented a case with tuberculous lymphadenopathy and immune-mediated thrombocytopenia, the complete remission with anti-tuberculous therapy, and partial response to immunoglobulin and steroid suggested a causal relationship between the two conditions.
Immune thrombocytopenic purpura is a diagnosis of exclusion, but many disorders like retroviral infections, autoimmune disorders, lymphoproliferative disorders, and primary immunodeficiency have been associated with this idiopathic disease. In children, the presentation is usually acute, but it can run a chronic course in adults (more than six months). Remission is considered if the platelets rise to 150�109, while a response is defined as platelets count above 50�109 or if there is a two-fold increase from the initial value [1,2]. Tuberculosis has re-emerged as a major health problem worldwide and can cause various hematological manifestations. Literature review documented few cases with isolated thrombocytopenia associated with tuberculosis [3,4]. We present a case of tuberculous lymphadenopathy with isolated thrombocytopenia.
A twenty-one-year Indian male shepherded presented to the emergency department with nose and gum bleeding for 2 days and skin rash on lower extremities for one day. The patient also reported painful, gradually increasing swelling on his lateral side of the upper neck during the last month associated with fever, chills, unexplained loss of weight, and sputum with streaks of blood and no bleeding from other sites. Systemic inquiries were unremarkable as were past (no history of hematological, rheumatic, or liver diseases) and family history, he was not taking any medications except for paracetamol. The patient is not consuming alcohol, recreational drugs, and not used to smoke.
�
The patient looks ill, oriented, and cooperative. Pallor was noted as were bleeding from gum, crust in his nostrils and extensive purpuric rash in his both lower limbs below the knee. There was no jaundice or cyanosis. Vital signs: Pulse 90/minute, blood pressure 126/65, respiratory rate 18/minute, and temperature 37.8. A lymph node 5�4 cm tender, firm, smooth surface, well defined, and mobile was found in the right submandibular region. Other lymph nodes were not palpable as were the liver and spleen.�
Admission full blood count showed: platelets of 5000, hemoglobin 9.9 grams/dl, and white cell count of 6.090. Neutrophils 3.41, lymphocytes 1.75, monocytes 0.46, and eosinophils 0.47, MCV 69.3, HCT 33.9, MCH 22.9, MCHC 33, RDWSD 39.2, and RDWCV 16. Investigations including liver (bilirubin, liver enzymes and serum albumin) lactate dehydrogenase (LDH), sputum for Acid Alcohol Fast Bacilli (AAFB), chest X-ray, abdominopelvic ultrasound, Combs�s test, renal functions, hepatitis B surface antigen Hepatitis C serology, HIV serology, antinuclear antibodies, PT, and APTT were all normal. The high sensitive C-Reactive Protein( CRP) was 13.2g/l (0-0.3).�
The blood picture suggests peripheral destruction. The patient started on methylprednisolone and immunoglobulin 40mg/kg body weight with partial improvement. Thus bone marrow biopsy was taken and showed: Normal erythrocyte series, leukocytes were normal in morphology and maturation with the blast in reasonable limits and reactive plasma cells, megakaryocytes were adequate with immature forms (Figure 1, Figure 2).�
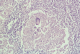
Excisional lymph node biopsy after unremarkable ENT and maxillofacial consultation was taken and revealed non-caseating granuloma diagnostic of tuberculous lymphadenopathy (Figure 3) and the patient was started, isoniazid, ethambutol, pyrazinamide, pyridoxine, and ciprofloxacin in the usual doses, with dramatic improvement, rifampicin was then introduced in place of ciprofloxacin. The discharge full blood count was: TWBCs 5800, hemoglobin 12g/dl, and platelets of 155000. The patient is now on regular follow up and is off specific treatment for immune thrombocytopenic purpura.
Immune thrombocytopenic purpura may require treatment with a steroid, immunoglobulins, and immunosuppressive therapy. Seventy percent of patients respond to treatment while a complete cure is observed in 20% of cases [1]. Tuberculosis can reduce platelets by various mechanisms: Antituberculous medications like rifampicin, ethambutol, and pyrazinamide, bone marrow involvement (granulomatosis, fibrosis, amyloidosis, and necrosis), hemophagocytic syndrome, hypersplenism, thrombotic thrombocytopenic purpura, and intravascular coagulation [5-11]. This patient showed a partial response to prednisolone and immunoglobulin, while he was completely cured with anti-tuberculous therapy and after three months not required specific treatment for ITP or splenectomy. Among the few cases reported in the literature with ITP in patients with complete tuberculosis, a response was observed during the first two months because the mycobacterium can remain alive during this period. Thus a causal relationship had been suggested, but the mechanism remains unknown [12-14].
�
In this report, the diagnosis of immune-mediated thrombocytopenia was diagnosed based on the following: 1) no previous drug therapy that can cause thrombocytopenia; 2) HIV, hepatitis viruses which can cause thrombocytopenia were excluded by the absence of clinical signs and negative investigations; 3) Lymphoproliferative and immunological disorders were not confirmed clinically together with normal bone marrow and negative anti-nuclear antibodies; 4) The healthy bone marrow also was against tuberculous infiltration and excluded hemophagocytic lymphohistiocytosis that had been previously linked to tuberculosis and can cause thrombocytopenia and anemia due to uncontrolled activation of T cells and macrophages, and an overproduction of inflammatory cytokines [15].�
The complete response to anti-tuberculous medication without the need for more specific medications for ITP and only partial response to these drugs confirm the causal relationship between ITP and tuberculosis.
Tuberculosis is a rare, treatable cause of thrombocytopenia that should be sought of especially among challenging to treat thrombocytopenia in the context of the clinical scenario. Relapse during treatment is not uncommon during the first months of treatment. Close monitoring and continuation of the particular therapy are of paramount importance.
The authors declare no competing interests.
All the authors contributed equally in the data collection and the drafting of the manuscript. All the authors read and agreed to the final manuscript.
Figure 1: bone marrow biopsy of the case report
Figure 2: bone marrow biopsy 40 magnification
Figure 3: lymph node tuberculosis of the reported case
- Cines DB, Blanchette VS. Immune thrombocytopenic purpura. N Engl J Med. 2002 Mar 28; 346(13):995-1008. PubMed | Google Scholar
- Cines DB, Bussel JB. How I treat idiopathic thrombocytopenic purpura (ITP). Blood. 2005 Oct 1; 106 (7):2244-51. PubMed | Google Scholar
- Goldenberg AS. Hematologic abnormalities and mycobacterial infections. In: Rom WN, Garay S, editor. Tuberculosis. New York, Litlle, Brown, and Comp; 1996. pp 645-655. Google Scholar
- Mert A, Bilir M, Tabak F, Ozaras R, Ozturk R, Senturk H, Aki H, Seyhan N, Karayel T, Aktuglu Y. Miliary tuberculosis: clinical manifestations, diagnosis, and outcome in 38 adults. Respirology. 2001; 6(3):217�224. PubMed | Google Scholar
- Glasser RM, Walker RI, Herion JC. The significance of hematologic abnormalities in patients with tuberculosis. Arch Intern Med. 1970 Apr; 125 (4):691-5. PubMed | Google Scholar
- Oyer RA, Schlossberg D. Hematologic changes in tuberculosis. In: Schlossberg D, editor. Tuberculosis &Nontuberculous Mycobacterial infections. 5th ed. New Delhi: Tata McGraw-Hill; 2007. pp 357-64. Google Scholar
- Maartens G, Willcox PA, Benatar SR. Miliary tuberculosis: rapid diagnosis, hematologic abnormalities and outcome in 109 treated adults. Am J Med. 1990 Sep; 89(3):291-6. PubMed | Google Scholar
- Ersley AJ. Hypersplenism and hyposlpenism. In: Williams WJ, Beutler E, Ersley AJ, Lichtman MA, editors. Hematology. 4th ed. New York: McGraw�Hill; 1990. p 695. Google Scholar
- Rosenberg MJ, Rumans LW. Survival of a patient with pancytopenia and disseminated coagulation associated with military tuberculosis. Chest. 1978 Apr; 73(4):536-9. Google Scholar
- Toscano V, Bontadini A, Falsone G, Conte R, Fois F, Fabiani A et al. Thrombotic thrombocytopenic purpura associated with primary tuberculosis. Infection.1995 Jan;23 (1):58-9. PubMed | Google Scholar
- Browett PJ, Varcoe AR, Fraser AG, Ellis-Pegler RB. Disseminated tuberculosis complicated by the hematophagocytic Syndrome. Aust N Z J Med. 1988 Feb; 18(1):79-80. PubMed | Google Scholar
- Al-Moamary MS, Black W, Bessuille E, Elwood RK, Vedal S. The significance of the persistent presence of acid-fast bacilli in sputum smears in pulmonary tuberculosis. Chest. 1999 Sep; 116 (3):726-31. PubMed | Google Scholar
- Ghobrial MW, Albornoz MA. Immune thrombocytopenia: a rare presenting manifestation of tuberculosis. Am J Hematol. 2001 Jun; 67(2):139-43. PubMed | Google Scholar
- Tsuro K, Kojima H, Mitoro A, Yoshiji H, Fujimoto M, Uemura M et al. Immune thrombocytopenic purpura associated with pulmonary tuberculosis. Intern Med.2006 Jul; 4(11):739-42. PubMed | Google Scholar
- Brastanios PK, Swanson JW, Torbeson M, Sperati J, Karakousis PC. Tuberculosis-associated haemophagocytic syndrome. Lancet Infectious Disease. 2006 Jul; 6(7):447-54. Google Scholar