Right ventricular outflow tract tachycardia worsened during pregnancy
Yibar Kambiré, Lassina Konaté, Georges Rosario Christian Millogo, Elodie Sib, Myriam Amoussou, Lucie Valérie Adélaďde Nebié, Ali Niakara
Corresponding author: Yibar Kambiré, Department of Medicine and Specialties, National Hospital Blaise Comparore, 11 PoBox 104 Ouagadougou, CMS 11, Burkina Faso 
Received: 02 Dec 2014 - Accepted: 05 Jan 2015 - Published: 22 Jan 2015
Domain: Clinical medicine
Keywords: Ventricular tachycardia, pregnancy, radiofrequency, Africa
©Yibar Kambiré et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Yibar Kambiré et al. Right ventricular outflow tract tachycardia worsened during pregnancy. Pan African Medical Journal. 2015;20:60. [doi: 10.11604/pamj.2015.20.60.5864]
Available online at: https://www.panafrican-med-journal.com//content/article/20/60/full
Right ventricular outflow tract tachycardia worsened during pregnancy
Yibar Kambiré1,&, Lassina Konaté1, Georges Rosario Christian Millogo2, Elodie Sib3, Myriam Amoussou4, Lucie Valérie Adélaďde Nebié3, Ali Niakara3
1Department of Medicine and Specialties, National Hospital Blaise Compaoré, 11 PoBox 104 Ouagadougou, CMS 11, Burkina Faso, 2Cardiology Department, Teaching Hospital Yalgado Ouedraogo, Ouagadougou, Burkina Faso, 3International Polyclinic of Ouagadougou, 01 BP 2092 Ouagadougou 01, Burkina Faso, 4Mother and Child Department, National Hospital Blaise Comparore, 11 PoBox 104 Ouagadougou, CMS 11, Burkina Faso
&Corresponding author
Yibar Kambiré, Department of Medicine and Specialties, National Hospital Blaise Comparore, 11 PoBox 104 Ouagadougou, CMS 11, Burkina Faso
We report the case of a 35 years old woman without underlying heart disease who was diagnosed with a right ventricular outflow tract tachycardia worsened during pregnancy. The diagnosis of ventricular tachycardia was made early in her pregnancy course but the patient had symptoms three months earlier. Her disease course was marked by rhythmic storms during the second trimester of pregnancy that led to three hospitalizations accounting for about two weeks in total. The combination of nadolol 80 mg and flecainide tablets 150 mg improved her rhythmic storms. Radiofrequency allowed a radical cure of this ventricular tachycardia. The patient is now asymptomatic 27 months after radiofrequency treatment.
Cardiac arrhythmia can occur during pregnancy in the presence or absence of an underlying organic heart disease. They are most often made of ventricular or supraventricular extrasystoles with a good prognosis. Sometime, they need treatment that can be difficult. We report the case of right ventricular outflow tract tachycardia worsened in pregnancy.
Mrs. AMS, 35 years old is seen at her outpatient visit on October 3, 2011 for a three months history of paroxysmal lipothymia occurring at rest, including while in bed and while driving her car. The episodes of lipothymia are accompanied by dizziness, light-headedness and short lasting blurred vision, all preceded by palpitations. There is neither dyspnea nor stress-related symptoms. Her cardiovascular risk factors are her overweight (BMI = 29.14 ) and an early death of her father at age 33 years due to kidney failure associated with hypertension. Her past medical history reveals asthma attacks that were treated as they occurred. Her last asthma attack happened over a year ago. She is primipara with a healthy child. The first episodes of palpitations occurred in July 2011 with a normal electrocardiogram. She was not pregnant then.
Cardiovascular examination is normal with a heart rate of 84 bpm, no heart murmur nor signs of heart failure. Blood pressure while lying down and standing up is 120/70 mmHg on her right arm and 110/60 mmHg on her left. Examination of other organs is normal. The 12-lead surface ECG is normal with regular sinus rhythm at 81 bpm and a normal adjusted QT interval. Doppler echocardiography is normal. Systolic function of both ventricles was preserved (LVEF = 70%; TAPSE = 23 mm). For instance, there is no left or right ventricular hypertrophy or dilation. 24-hoursHolter ECG shows a sinus rhythm at 88 bpm without rhythm or conduction disorders. Her electrolytes, creatinine, blood count, blood glucose and ultra- sensitive TSH are normal except for hypomagnesemia at 0.50 mmol. She is prescribed six tablets a day of magnesium for a week, and atenolol 25 mg per day. Driving is not recommended. A control of her metabolic panel, realized on November 3, 2011 is normal.
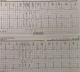
Her lipothymia symptoms reoccurred on November 22, 2011, after a three weeks amendment. A 24-hours Holter ECG performed on November 23, 2011 is in sinus rhythm at 96 bpm, revealed many ventricular extrasystoles with R/T phenomenon. These extrasystoles included 30 doublets and six attacks of unsustained ventricular tachycardia (VT). She is prescribed amiodarone 200 mg daily which is quickly replaced by atenolol 50 mg and 100 mg causing the symptoms to subside. On January 25th, 2012, she reported chest tightness lasting less than a minute without palpitations or lipothymia. The patient is two months pregnant. Cardiac examination is normal. Troponin is negative and lipid profile is normal. Atenolol treatment is continued at 100 mg/day. On March 26th, 2012, Mrs. AMS is four months pregnant and is admitted to the emergency room for lipothymia, discomfort, and dizziness preceded by palpitations. She is anxious. Cardiac examination and blood pressure are normal. Pregnancy has a normal course. A surface ECG (Figure 1) records a monomorphic VT attack such as a left conduction slowness that was unsustained but rapid. Thyroid hormones, blood electrolytes, glucose, creatinine and blood count were normal. She was hospitalized in intensive care under ECG monitoring through a scope that recorded many unsustained VT attacks. Her treatment consisted potassium chloride, magnesium sulfate through an electric pump, the substitution of 100 mg atenolol by 200 mg acebutolol, and enoxaparin for primary prevention of venous thromboembolic disease.
Ventricular tachycardia attacks persisted under this treatment. Replacement of acebutolol by nadolol brought her back to normal sinus rhythm and she was discharged on the third day of hospitalization. An outpatient Holter ECG was performed on 03/28/2012 recorded ventricular extrasystoles numerous unsustained VT attacks (Figure 2) and rare supraventricular extrasystoles. She is readmitted on March 30th, 2012, for the same symptoms. A Holter ECG revealed frequent monomorphic ventricular extrasystoles (1287) of which 318 unsustained VT attacks. The combination of 100 mg flecainide (1/2 tablet three times per day) with 80 mg nadolol (1/4 tablet twice ŕ day) controlled the arrhythmia and she was discharged on the tenth day of hospitalization. Under this treatment and oral solution of magnesium sulfate a Holter ECG monitoring revealed a marked improvement in monomorphic ventricular extrasystoles with only three doublets and one unsustained ventricular attack. Mrs. AMS is then transferred to another country where advanced technology electrophysiological study confirmed the infundibular type of her VT. She is successfully treated with radiofrequency ablation. Antiarrhythmic drugs are discontinued. At 27 months post-ablation Ms. AMS is doing well. She has had a vaginal delivery of a full term healthy child with no cardiac complication before undergoing radiofrequency.
Cardiac arrhythmias can occur during pregnancy in the presence or absence of an underlying organic heart disease [1,2]. They are most often made of ventricular or supraventricular extrasystoles with a good prognosis. The mechanisms of these arrhythmias include hemodynamic changes during pregnancy, the main ones being an increase in total blood volume, an increase in heart rate inducing an increase in cardiac output and the decrease in peripheral arterial resistance [1] but also the intrinsic severity an underlying heart disease. The increase in heart rate is related to sympathetic stimulation, stress, pregnancy, hormonal phenomena and could generate cardiac arrhythmias [3].
Right ventricular outflow tract tachycardia on its own is a rhythm disturbance occurring on hearts that are usually healthy and it has good prognosis [3]. It is not specific to pregnancy and is most often seen in young women. Is the association with pregnancy a coincidence? This assumption is plausible in our case since the patient presented similar symptoms three months prior to the diagnosis of arrhythmias and prior to pregnancy. As a matter of fact, the recurrence of symptoms led to her outpatient visit to our hospital. It is known that ventricular tachycardia may be revealed or worsened by pregnancy [1,4]. Although the association is fortuitous, the severity of the right ventricular outflow tract tachycardia remains a key question. Indeed several hospitalizations were required with a relative resistance to antiarrhythmic drugs (atenolol alone, acebutolol). The causes of ventricular tachycardia during pregnancy are multiple [1,4-7] including peripartum cardiomyopathy, congenital heart disease that are operated on or unknown, and other types of heart diseases. In the case of the right ventricular outflow tract tachycardia, it is often a VT on a healthy heart. In our case, the absence of echocardiographic abnormalities, the absence of abnormal QT and a normal QRS morphology caused us to suggest right ventricular outflow tract tachycardia. Although the prognosis is generally benign, the persistent symptoms despite numerous medications, the heart rate that was accelerated at times, the psychological impact and the history of premature death of the father led us to want to rule out any unknown cause. Electrophysiological studies were not possible in a resource-limited setting. The effective combination therapy has been the association nadolol 80 mg and flecainide 150 mg. Ultimately radiofrequency performed after medical transfer allowed proper diagnosis and ideal therapy. The course of the disease brought satisfaction and a happy outcome for the pregnancy and the mother despite rhythmic storms. This is the classic trend of the association "ventricular tachycardia on a healthy heart-pregnancy". Treatment is made of medical antiarrhythmic such as beta-blockers, verapamil, procainamide, and flecainide in the vast majority of cases [5,8-12]. Ajmaline, procainamide or lidocaine are used in well tolerated cases but external electrical cardioversion is used in case of hemodynamic instability [12,13]. Exceptionally the implantable automatic defibrillator is indicated for secondary prevention of sudden death in the presence of syncope or resuscitation due to ventricular tachycardia, ventricular fibrillation or ventricular flutter [13]. In our case, a resource-limited context, unpleasant symptoms for the patient, very rapid ventricular rhythms at times, have led us to transfer our patient for electrophysiological tests, then radiofrequency ablation. The postoperative course was uneventful and the patient remained asymptomatic 27 months after without antiarrhythmic drugs.
This case brings forth the problematic issue of tachycardia associated with pregnancy and specifically the issue of optimal management of conventional drugs resistant cases through interventional cardiology in developing countries.
Authors declare no competing interest.
Y. Kambiré: Lead author handled the case, collected the data and wrote the article. L. Konaté, GRC Millogo, E. Sib, M. Amoussou, LVA Nebié and A. Niakara: participated in the management of case and corrected the article. All authors have read and approved the final manuscript.
The authors thank Dr Maxime Firmin Toé for his participation in the management of the case; Drs. Caled Tindano and Theodore Boro for the translation of this article in English.
Figure 1: electrocardiogram of a 4 month pregnant woman showing two unsustained ventricular tachycardia attack on lead II
Figure 2: unsustained ventricular tachycardia on a 24-hours Holter ECG tracing of a patient during pregnancy
- Dawn Adamson L, Catherine Nelson-Piercy. Managing palpitations and arrhythmias during pregnancy. Heart. 2007;93(12):1630-1636. PubMed | Google Scholar
- Samuel C Siu, Mathew Sermer, Jack M Colman, A Nanette Alvarez, Lise-Andree Mercier, Brian C Morton, Catherine M Kells, M Lynn Bergin, Marla C Kiess, Francois Marcotte, Dylan A Taylor, Elaine P Gordon, John C Spears, James W Tam, Kofi S Amankwah, Jeffrey F Smallhorn, Dan Farine, Sheryll Sorensen. On behalf of the Cardiac Disease in Pregnancy (CARPREG) Investigators: Prospective multicenter study of pregnancy outcomes in women with heart disease. Circulation. 2001;104:515-521. Google Scholar
- Mikiko Nakagawa, Sayo Katou, Masashi Ichinose, Seiki Nobe, Hidetoshi Yonemochi, Isao Miyakawa, Tetsunori Saikawa. Characteristics of New-Onset Ventricular Arrhythmias in Pregnancy. J Electrocard. 2004;37(1):47-53. PubMed | Google Scholar
- Rouslan Kotchetkov, Ameen Patel, Omid Salehian. Ventricular Tachycardia in Pregnant Patients. Clin Med Insights Cardiol. 2010; 4: 39-44. PubMed | Google Scholar
- John Abboud, Yahya Murad, Carol Chen-Scarabelli, Louis Saravolatz, Tiziano M Scarabelli. Peripartum cardiomyopathy: a comprehensive review. Int J Cardiol. 2007;118(3):295-303. PubMed | Google Scholar
- Gail D Pearson, Jean-Claude Veille, Shahbudin Rahimtoola, Judith Hsia, Celia M Oakley, Jeffrey D Hosenpud, Aftab Ansari, Kenneth L Baughman. Peripartum cardiomyopathy: National Heart, Lung, and Blood Institute and Office of Rare Diseases (National Institutes of Health) workshop recommendations and review. JAMA. 2000;283:1183-1188. Google Scholar
- Koichiro Niwa, Shigeru Tateno, Teiji Akagi, Wakako Himeno, Yasutaka Kawasoe, Shunsuke Tatebe, Kozo Matsuo, Michael A Gatzoulis, Makoto Nakazawa. Arrhythmia and reduced heart rate variability during pregnancy in women with congenital heart disease and previous reparative surgery. Int J Cardiol. 2007;122(2):143-148. PubMed | Google Scholar
- Deborah Wolbrette. Treatment of arrhythmias during pregnancy. Curr Womens Health Rep. 2003;3(2):135-139. PubMed | Google Scholar
- Nisha Chibber Chandra, Elena A Gates, Mahmud Thamer. Conservative Treatment of Paroxysmal Ventricular Tachycardia During Pregnancy. Clin Cardiol. 1991;14(4):347-350. PubMed | Google Scholar
- Ying-Chi Hsu, Ya-Pei Chen. Right Ventricular outflow Tract (ROVT) Ventricular Tachycardia (VT) in Pregnancy : A Case Report. Intern Med. 2010; 21:140-143. Google Scholar
- Hans-Joachim Trappe. Cardiac Arrythmia in The Pregnant Woman and the fœtus. Eur Cardiol Rev. 2008;4(2):67-71. PubMed | Google Scholar
- Michael Brodsky, Robert Doria, Byron Allen, David Sato, Gregory Thomas, Mark Sada. New-onset ventricular tachycardia during pregnancy. Am Heart J. 1992;123(4Pt 1):933-941. PubMed | Google Scholar
- Hans-Joachim Trappe. Arrhythmias during pregnancy. Dtsch Med Wochenschr. 2008;133(36):1799-1804. PubMed | Google Scholar