Spectrum of intracranial tumours in a tertiary health care facility: our findings
Sunday Sokunle Soyemi, Olugbenga Olayide Oyewole
Corresponding author: Sunday Sokunle Soyemi, Department of Pathology and Forensic Medicine, Lagos State University Teaching Hospital, Ikeja, Lagos, Nigeria, Department of Oncology, Lagos State University Teaching Hospital, Ikeja, Lagos, Nigeria 
Received: 01 Jul 2014 - Accepted: 02 Sep 2014 - Published: 09 Jan 2015
Domain: Epidemiology
Keywords: Magnetic resonance imaging, intracranial, WHO
©Sunday Sokunle Soyemi et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Sunday Sokunle Soyemi et al. Spectrum of intracranial tumours in a tertiary health care facility: our findings. Pan African Medical Journal. 2015;20:24. [doi: 10.11604/pamj.2015.20.24.4935]
Available online at: https://www.panafrican-med-journal.com//content/article/20/24/full
Spectrum of intracranial tumours in a tertiary health care facility: our findings
Sunday Sokunle Soyemi1,2,&, Olugbenga Olayide Oyewole1
1Department of Pathology and Forensic Medicine, Lagos State University Teaching Hospital, Ikeja, Lagos, Nigeria, 2Department of Oncology, Lagos State University Teaching Hospital, Ikeja, Lagos, Nigeria
&Corresponding author
Sunday Sokunle Soyemi, Department of Pathology and Forensic Medicine, Lagos State University Teaching Hospital, Ikeja, Lagos, Nigeria, Department of Oncology, Lagos State University Teaching Hospital, Ikeja, Lagos, Nigeria
Introduction: primary brain tumours are uncommon with an annual incidence of 5-10/100000. This study has attempted to analyse the histological pattern of intracranial tumours seen in our centre.
Methods: a retrospective study of cases of intracranial tumours seen was conducted over a period of 5 years ie from January 2008 to December 2012. All the slides were reviewed. The age, sex, diagnosis using the WHO grading and the histological subtypes were recorded. Data were analysed using the (SPSS) Software version 17.
Results: altogether, 56 cases of intracranial tumours were seen out of a total of 12,610biopsies representing 0.004% .The male to female ratio (M: F) was approximately 1:1.1The mean age of the patients was 36 � 20.35 (range, 2 to 85). Astrocytomas accounted for 30% (17)while 29% (16) had Meningioma.Medulloblastoma accounted for 18%.(10).Of the cases of Gliomas, majority(52%) fell under WHO grade II. (38%)of the Meningioma were of the mixed type while 25% had transitional type.
Conclusion: astrocytomas was the commonest brain tumour.These patterns corroboratedmost studies that have been done.Metastasis to the brain was however, not seen in this study.
During embryogenesis the neuroectoderm differentiates into the neuroepithelium from which three primitive tissue are derived namely; the neuroblast, thespongioblast and the primitive ependymal cells. Intracranial neoplasms may arrive at any level of differentiation of these cells [1]. Brain tumours are a diverse group of primary CNS tumours and secondary neoplasms arising either from the brain or from haematogenous spread from distant sites. Each tumour has a distinctivebiology, treatment and prognosis [2].
�
The annual, global, age standardized incidence of primary malignant intracranial tumours is approximately 3.7 per 100,000 for males and 2.6 per 100,000 for females [3,4]. Gliomas are common tumours in adults and paediatric age group. In the adult population, Anaplastic Astrocytoma and Glioblastoma Multiforme are the most common glial tumours with an annual incidence of 3 to 4 per 100,000 populations [5]. Although few studies had been done on the epidemiology of intracranial tumours in Nigeria and Africa as a whole, the objective of this paper is to provide an ample and detailed perspective on the epidemiological studies of intracranial tumour in a newly growing tertiary health facility in Lagos, Nigeria.
A retrospective study of cases of intracranial tumours seen was conducted over a period of 5 years ie from January 2008 to December 2012. These were Nigerian patients who had surgery and their samples were sent to our histopathology department for diagnosis. The total sample seen over this period was relatively small when compared to other studies. This was due to the fact that the neurosurgery department was new and had only one neurosurgeon.The specimens were processed in paraffin and stained with eosin and haematoxylin. In rare cases special stains were used to demonstrate neuroglial cells, reticulin and collagen fibres.All the slides were reviewed. The age, sex, diagnosis using the WHO grading and the histological subtypes were recorded. Data were analysed using the (SPSS) Software version 17.
Altogether, 56 cases of intracranial tumours were seen out of a total of 12,610 biopsies representing 0.004% of the surgical biopsies. The male to female ratio (M: F) was approximately 1:1.1. The mean age of the patients was 36 � 20.35 (range, 2 to 85). Astrocytomas accounted for 30% (17), 29% (16) had Meningioma while Medulloblastoma accounted for 18%. Pituitary adenoma and Ependymomas represented 14% and 9% respectively (See Table 1). Of the cases of Astrocytic tumours, (Table 2) majority (52.9 %) fell under WHO grade II this is followed by Glioblastoma Multiforme which represented 35.2%. In Table 3, 37.5% of the Meningiomas were of the mixed type while 25% had transitional type.Meningothelial, Fibroblastic and Psammomatous each had 12.5%.
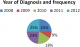
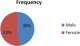
In this study, the lowest cases were seen in year 2009 while the highest were seen in 2008 and 2012 (Figure 1). The male to female ratio was 1:1.1 with no significant gender difference (Figure 2). Other studies have reported insignificant gender difference [1,2].The peak age of occurrence in adult was 21-30 years with only seven cases seen in children. Only one case of intracranial tumour was seen in person above 70 years. This is closely compatible to a similar study done over an eleven year period in Ibadan, South West Nigeria [6] ie from 1980 to 1990 which revealed a ratio of 1:1. However a twist is seen in the high occurrence of metastatic tumours which came next to Astrocytoma in the same study done by Olasode in Ibadan, Nigeria.
�
In our study, no single case of metastasis to the brain was found. The reason may likely be due to the relatively small numbers (56) compared to the study in Ibadan (210) of eleven years duration. Early detection of cancers by newer diagnostic methods and sophisticated treatment options in this decade compared to the last two decades might also be a contributing factor for the absence of intracranial metastasis. In this study Astrocytoma was the most common intracranial tumour. Other studies have also revealed the predominant nature of Astrocytoma [7-10].�
Meningiomas have been found to be high in Africans and constitute approximately 20% of intracranial tumours [10]. In our study, it accounted for 29%. This figure is relatively higher than other previous works [9-11] although closely compatible with a similar study in Iran [12] and in Egypt [13]. It is worthy of note that an unequivocal factor that has been implicated in Meningioma is irradiation of the cranium even at low doses [14,15].�
Some other studies which have tried to establish a relationship between the development of brain neoplasm and head injuries, exposure to high tension wires, use of cellular phones and dietary exposure to N-nitrosoureas are really not convincing and are also controversial [16-19] .The changing trend in meningioma and it�s associated hypothesis would presently serve as an area of future research that can be prioritized.�
One of the most common tumours of the posterior fossa is Medulloblastomas which is highly invasive. This tumour also has a high tendency to recur and spread through the CSF space, subsequently making radical cure of the tumour a problem [2]. In this study, it accounted for 18%. This is compatible with most Caucasian studies where itaccounts for 12-25% of all paediatric CNS tumours [20].�
Pituitary adenoma constituted 14% of all tumours. This is compatible with similar studies done in Ghana [11] Egypt [13] and Nigeria [6,9,11].
In conclusion, astrocytoma and meningioma are the most common intracranial tumours in our study.
The authors declare no competing interests.
SSS is a lecturer and consultant pathologist who performed the literature search and prepared the manuscript. OOO extracted the data from the records. All authors read and agreed to the final version of this manuscript and equally contributed to its content and to the management of the case.
We thank the histotechnologist who prepared the slides in cases where they were broken. We are grateful to the department for given us the approval to report this case.
Table 1: frequency and percentage distribution of the different types of tumour
Table 2: percentage distribution of the different grades of Astrocytoma
Table 3: frequency and percentage distribution of the different types of meningioma seen I this study
Figure 1: distribution of the frequency in each year from 2008 to 2012
Figure 2: male to female distribution of the intracranial tumours
- Olasode BJ,Shokunbi MT, Aghadiuno PU. Intracranial neoplasms in Ibadan, Nigeria.East Afr Med Journal. 2000; 77(1):4-8. PubMed | Google Scholar
- Idowu O, Akang E, Malomo A. Symptomatic primary intracranial neoplasm in Nigeria. West Afri. J NeurolSci (Turk) 2007;19(24):212-218. PubMed | Google Scholar
- GLOBOCAN.Worldwide incidence and mortality of cancer,2002 (Computer programm),Lyon, France: IARC Press; 2002. Google Scholar
- Parkin DM, Whelan SL, Ferlay J, Teppo L, Thomas DB. Cancer in five continents, Vol 5. Lyon, France: IARC Press; 2002. Google Scholar
- De Angelis LM. Brain tumours. N Engl J Med. 2001 Jan 11;344(2):114-23. PubMed | Google Scholar
- Olasode BJ. A pathological review of intracranial tumours seen at the University College Hospital, Ibadan between 1980 and 1990. Niger Postgrad Med J. 2002;9(1):23-8. PubMed | Google Scholar
- Shah SH, Soomro IN, Hussainy AS, Hassan SH. Clinico-pathological pattern of intracranial tumours in children. J Pak Med Assoc. 1999;49(3):63-5. PubMed | Google Scholar
- Mwangombe NJ, Ombachi RB. Brain tumours at the Kenyatta National hospital, Nairobi. East Afr Med J. 2006;77(8):444-7. PubMed | Google Scholar
- Ohaegbulam SC, Saddeqi N, Ikerionwu S.Intracranial tumours in Enugu, Nigeria. Cancer. 1980; 46(10):2332-2334. PubMed | Google Scholar
- Jackson JG, Okubadejo GA. A review of intracranial tumours seen in necropsies at the University College Hospital, Ibadan between 1957 and 1961. West Afr Med J. 1963;12:251-263. PubMed | Google Scholar
- Adeloye A. Neoplasms of the brain in the Africans. Surg Neurol. 1970; 11:247-255. PubMed | Google Scholar
- Mehrazin M, Rahmat H, Yavari P. Epidemiology of primary intracranial tumours in Iran, 1978-2003. Asian Pac J Cancer Prev. 2006;7(2):75-7. PubMed | Google Scholar
- Sorour O, Rifaat M, Loft C. The relative frequency of brain tumour in Egypt. Afr J Med Sci. 1973 Apr;4(2):178-86. PubMed | Google Scholar
- Pollak L, Walach N, Gur R, Schiffer J. Meningiomas after radiotherapy for tineacapitis ? still no history. Tumori. 1998 Jan-Feb;84(1):65-8. PubMed | Google Scholar
- Walter AW, Hancock ML, Pui CH, et al. Secondary brain tumors in children treated for acute lymphoblasticleukemia at St Jude Children's Research Hospital. J Clin Oncol. 1998 Dec;16(12):3761-7. PubMed | Google Scholar
- Inskip PD, Mellemkjaer L, Gridley G, Olsen JH. Incidence of intracranial tumors following hospitalization for head injuries (Denmark). Cancer Causes Control. 1998 Jan;9(1):109-16. PubMed | Google Scholar
- Salvatore JR, Weitberg AB, Mehta S. Nonionizing electromagnetic fields and cancer: a review. Oncology (Williston Park). 1996 Apr;10(4):563-70. PubMed | Google Scholar
- Inskip PD, Tarone RE, Hatch EE, et al. Cellular-telephone use and brain tumors. N Engl J Med. 2001 Jan 11;344(2):79-86. PubMed | Google Scholar
- Kaplan S, Novikov I, Modan B. Nutritional factors in the etiologyof brain tumors: potential role of nitrosamines, fat, and cholesterol. Am J Epidemiol. 1997 Nov 15;146(10):832-41. PubMed | Google Scholar
- Farwell JR, Dohrmann GJ, Flannery JT. Medulloblastomain childhood: an epidemiological study. J Neurosurg. 1984 Oct;61(4):657-64. PubMed | Google Scholar