Ossified chronic epidural hematoma of the posterior fossa
Ali Akhaddar, Omar Boulahroud
Corresponding author: Ali Akhaddar, Department of Neurosurgery, Avicenne Military Hospital, Marrakech, Morocco 
Received: 03 Feb 2014 - Accepted: 21 Oct 2014 - Published: 13 Mar 2015
Domain: Clinical medicine
Keywords: Chronic, epidural hematoma, posterior fossa
©Ali Akhaddar et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ali Akhaddar et al. Ossified chronic epidural hematoma of the posterior fossa. Pan African Medical Journal. 2015;20:238. [doi: 10.11604/pamj.2015.20.238.3954]
Available online at: https://www.panafrican-med-journal.com//content/article/20/238/full
Ossified chronic epidural hematoma of the posterior fossa
Ali Akhaddar1,2,&, Omar Boulahroud3
1Department of Neurosurgery, Avicenne Military Hospital, Marrakech, Morocco, 2University of Mohammed V Souissi, Rabat, Morocco, 3Department of Neurosurgery, Mohammed V Military Teaching Hospital, Rabat, Morocco
&Corresponding author
Ali Akhaddar, Department of Neurosurgery, Avicenne Military Hospital, Marrakech, Morocco
A 15-year-old adolescent presented to us with mild headache, progressive dizziness and recent vomiting since 2 weeks without seizures. There was a history of head injury (neglected) following a stone-throwing incident 2 months earlier. On examination, he was conscious with a left cerebellar syndrome but without other neurologic deficit. Routine biologic data were normal. CT-scan revealed left posterior fossa extradural lesion with hypodensity in the center and calcified wall (A). MRI showed that the lesion was liquid with homogeneous ring enhancement following gadolinium injection and cerebellar compression (B and C). A sub-occipital craniotomy was done and a chronic liquefied hematoma was removed. There was a thick hard calcified wall relatively adherent to the duramater (D). Postoperative period was uneventful and the patient was discharged symptoms free. Histologically, the wall contains large areas of ossification. Ossified chronic epidural hematoma is a very rare complication following head injury. The blood accumulates slowly from a venous source becomes chronic extradural hematoma and becomes calcified or ossified due to an inflammatory reaction of the dura especially in children. This rare phenomenon should be considered in the differential diagnosis of other traumatic epidural and subdural hematomas.
Figure 1: Axial CT-scan. (A): revealing a left posterior fossa chronic extradural biconvex lesion with ossified wall (arrow). MRI: Axial T1-weighted image after gadolinium injection; (B): T2-weighted image; (C): fluid-liquid lesion with homogeneous ring enhancement and significant cerebellar compression; (D): operative view demonstrating the ossified wall (arrow) after superficial dissection from the duramater
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
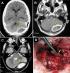 Figure 1: Axial CT-scan. (A): revealing a left posterior fossa chronic extradural biconvex lesion with ossified wall (arrow). MRI: Axial T1-weighted image after gadolinium injection; (B): T2-weighted image; (C): fluid-liquid lesion with homogeneous ring enhancement and significant cerebellar compression; (D):Operative view demonstrating the ossified wall (arrow) after superficial dissection from the duramater
Figure 1: Axial CT-scan. (A): revealing a left posterior fossa chronic extradural biconvex lesion with ossified wall (arrow). MRI: Axial T1-weighted image after gadolinium injection; (B): T2-weighted image; (C): fluid-liquid lesion with homogeneous ring enhancement and significant cerebellar compression; (D):Operative view demonstrating the ossified wall (arrow) after superficial dissection from the duramater