An unusual presentation of carcinoma stomach
Jeffey George, Deepak Kochummen Johnson, Rajneesh Anugraha Rajan, Sandesh Kolassery, Ramachandran Mavali Thazhath
Corresponding author: Thazhath Mavali Ramachandran, Dept of gastroenterology, medical college, Calicut, Kerala India 
Received: 07 Sep 2011 - Accepted: 23 Jun 2012 - Published: 05 Mar 2013
Domain: Clinical medicine
Keywords: Adenocarcinoma stomach, dic, bone metastasis
©Jeffey George et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Jeffey George et al. An unusual presentation of carcinoma stomach. Pan African Medical Journal. 2013;14:84. [doi: 10.11604/pamj.2013.14.84.1203]
Available online at: https://www.panafrican-med-journal.com//content/article/14/84/full
An unusual presentation of carcinoma stomach
Jeffey George1, Deepak Kochummen Johnson1, Rajneesh Anugraha Rajan1, Sandesh Kolassery1, Ramachandran Mavali Thazhath1,&
1Department of gastroenterology, medical college, Calicut, India
&Corresponding author
Thazhath Mavali Ramachandran, Dept of gastroenterology, medical college, Calicut, Kerala India
Symptomatic gastric malignancy usually presents with symptoms which mimic peptic ulcer disease.Usual presenting features include weight loss and abdominal pain. Other symptoms include nausea, vomiting, dysphagia, melena and early satiety. Gastric malignancy presenting with hemetemesis, macular skin lesions of DIC and low backache due to bone metastasis from the primary is rare. Also bone metastasis in gastric cancer in the absence of hepatic metastasis is also rare.
Gastric malignancy can have protean manifestations. We present a rare manifestation of adenocarcinoma of stomach in a young patient.
A 33-year man working in Gulf, presented with hemetemesis 15 days ago in the month of February this year. This was preceeded by low grade fever, bone pain ,generalised bodyache, low back ache and generalised macular skin rashes. There was no history of abdominal pain, jaundice or features of chronic liver disease.He gave history of intake of analgesics for backache. After symptomatic treatment he returned back. He came to our OPD with Complete blood count which showed a haemoglobin of 8g/dl, total count 6700/mm3 platelet count 24000/mm3 and ESR 55mm/hr. On examination patient was pale with non pruritic macular rashes and mild splenomegaly.Residing in Middle East with background history of fever, backache, skin rash, splenomegaly and a low platelet count possibility of atypical infection like Brucellosis with NSAID induced gi bleed was considered.
He was admitted for further evaluation and endoscopy done showed a nodular ulcerative lesions in the antrum of stomach and histopathologic examination confirmed adenocarcinoma of stomach (Figure 1, Figure 2, Figure 3). Liver function tests showed a high ALP (1536 U/l), elevated INR (2.15) though bilirubin, transaminases and serum proteins were normal. Brucella agglutination test was negative. Xray Chest was normal. Ultrasound of abdomen showed normal echotexture of liver, no SOL, normal portal vein and no IHBRD. CT scan of the abdomen revealed gross pylorus thickening with regional lymphadenopathy and skeletal metastasis with sclerotic foci involving vertebrae and pelvic bones and lytic areas in bilateral iliac blades with no liver metastasis or ascites. A skeletal survey was done which showed lytic lesions in the iliac and femoral bones. Bone marrow aspirate showed decreased red cells and platelets and marrow biopsy done was reported as metastasis from adenocarcinoma (Figure 4). Coagulation profile done was suggestive of DIC due to the raised levels of FDP (5,170 ng/dl ) and a low fibrinogen(152mg/dl).
He was transferred to Medical Oncology department for subsequent management and was treated with chemotherapy. He succumbed to his illness within 10 months of diagnosis.
This young patient had adenocarcinoma stomach with bone metastasis , marrow infiltration and DIC in the absence of liver metastasis. Bone metastasis are classically associated with carcinoma of thyroid, kidney, lung and prostrate. Bone metastasis occurs in only 0- 17% of cases of gastric carcinoma [1] which can be either osteosclerotic or osteolytic [2]. In this case there was no involvement of liver which points to a non portal spread of the tumor probably via Batsons plexus [3] which explains the distant metastasis in the absence of liver metastasis. Apart from bone metastasis the patient also had evidence of Disseminated intra vascular coagulation.The incidence of DIC ranges from 10 - 75 % [4] . DICobserved in advanced cancer patients is due to acute or gradual development of fibrin microthrombi which may be due to multiple factors such as direct endothelial injury, coagulation cascade activation, production of procoagulant substances and reduction in the synthesis or activity of anticoagulant factors. Eventhough coagulation abnormality can occur in carcinoma stomach due to various factors clinically manifest DIC as in this patient is rare [5,6] Reports of adenocarcinoma stomach presenting as DIC are usually associated with large tumor burden and metastasis [4].
Gastric neoplasm should be considered in the differential diagnosis of metastatic bone lesions with unknown primary. Rarely DIC can be the presenting feature of stomach malignancy.
The authors declare that they have no competing interests
Jeffey George worked up the case, drafted the article, Deepak Kochummen, Johnson assisited in the workup, Rajneesh Anugraha Rajan assisited in the workup, Sandesh Kolassery drafted the article, Ramachandran Mavali Thazhath drafted the article, critical review. All the authors have read and approved the final version of the manuscript.
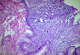
Figure 1: Adenocarcinoma stomach( above) low power showing tumor cells diffusely and a vague glandular pattern composed of cells with hyperchromatic and pleomorphic nuclei and prominent nucleoli
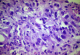
Figure 2: (below) high power showing glands lined by cells having pleomorphic vesicular nuclei with prominent nucleoli
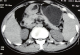
Figure 3: Adenocarcinoma stomach -CT scan of abdomen showing gross thickening of pylorus with regional lymphadenopathy suggestive of advanced gastric malignancy
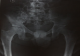
Figure 4: Xray AP pelvis showing lytic bone lesions in the right femur
- Mohandas MK, Swaroop SV, Krishnamurthy S, Desai CD, Dhir V, Pradhan AS et al. Unusual bone metastasis as the initial symptom of gastric cancer - a report of four cases. Indian J Cancer. 1993; 30:146-50. PubMed | Google Scholar
- Carstens SA, Resnick D. Diffuse sclerotic skeletal metastasis as an initial feature of gastric carcinoma. Arch Intern Med. 1980; 140:1666-8. PubMed | Google Scholar
- Sagara K, Fujiyama S, Kin F, Sato T. An unusual case of Gastric corcinoma initially presenting bone metastasis and later transverse myelopaty. Jpn J Clin Oncol. 1985 Mar; 15(1):133-4. Google Scholar
- Colman R W, Rubin R N. Disseminted intravascular coagulation due to malignancy. Semin Oncol. 1990; 17:172-86. PubMed | Google Scholar
- Deshpande AA, Gandhi JA, Shetty G, Deshmukh S, Joshi AS, Hardikar JV. Gastric cancer presenting with acute disseminated intravascular coagulation. Indian J Gastroenterol. 2002 Jul-Aug; 21(4):164-5. PubMed | Google Scholar
- Fung WP, Barr AV. Fulminant disseminated intravascular coagulation in advanced gastric carcinoma. Am J Gastroenterol. 1979 Feb; 71(2):210-2. PubMed | Google Scholar